The first sign of genetic hair loss in men is often a bit of recession at the temples, or a little thinning in the crown. One may notice a subtle change in the texture of the hair at the hairline, or have the perception that one’s hair feels less full overall. However, the experience of having large amounts of hair suddenly appear on the comb, brush or pillow, is generally not a sign of hereditary baldness.
In hereditary baldness — which also goes under the name of male pattern hair loss, androgenetic alopecia, androgenic alopecia, and common baldness — healthy, full-thickness terminal hair is gradually replaced by finer, shorter hair. As we saw in a previous chapter, this process, called “miniaturization,” is caused by the action of DHT on the hair follicle. Besides causing the hair to miniaturize, DHT also shortens the hair cycle so that hair that is at the end of its cycle is replaced by new, finer hair – each time at a slightly faster rate. The shortened hair cycle may contribute to the perception of slightly more hair falling out, but there is no significant shedding associated with common balding.
To say it another way, male pattern baldness is not a condition where hair falls out in mass, but rather a condition where full thickness terminal hair is gradually replaced by finer, miniaturized hair. At some point the DHT-affected hair will become so fine, that it will have no cosmetic value and the area will appear bald. Common baldness, therefore, is a process of hair “thinning” that only at its end stage leads to actual hair “loss”.
Men who are going to become very bald usually see the first signs of hair loss in their late teens and early twenties. The younger the age that a person begins to thin, the more extensive the hair loss is likely to become. If a man passes though the twenties with no hair loss, it is unlikely (thought not impossible) that he will become very bald. Dark-haired men, particularly those with light skin, will generally notice hair loss earlier than light-haired men do, but the rate of hair loss is no different.
At the first signs of balding, some people panic, some become depressed, and others resort to using potions, shampoos, or other over-the-counter remedies. Possibly the worst choice would be to try to get a quick fix through surgery.
So if you think you are losing your hair, what should one do? Don’t panic! Consider these three simple things:
- Decide if the hair loss really bothers you.
This may seem like a silly comment but, in fact, hair loss doesn’t bother everyone. Some people just accept it and move on. If it does bother you, that is O.K. too. You should not feel bad or guilty about it, even if your response seems a bit excessive. It is common for people to be worried, concerned, and even depressed, when they think they are losing their hair. - Diagnose the cause.
Before running to the store and buying an armful of hair loss remedies, have a consultation with a board certified dermatologist (these are the doctors whose specialty includes the diagnosis of hair loss) to have an accurate diagnosis made. If you don’t know any in your area, you may find one through the American Academy of Dermatology www.AAD.org. As we saw in a previous chapter, there are numerous causes of hair loss, many of them treatable, and the diagnosis is not always clear cut. A thorough medical history and examination of the hair and scalp by a professional can secure the diagnosis. - Consider medical treatments before surgery.
Particularly when androgenetic hair loss is in its early stages, medications are the treatment of choice. Not only can prescription drugs, like finasteride (Propecia), slow or prevent further hair loss, they can actually grow hair back if started when the process is just beginning. Other treatments, such as changing hair styles and cosmetic camouflage, can also be useful in certain situations.
As a rule, you should always begin drug therapy early and have surgery late – after non-surgical options have been exhausted. It is a poor argument “to start surgery early, so that no one will notice” or to use surgery as prevention for hair loss. These strategies only serve the hair transplant surgeon, not the patient. Hair transplant surgery should not be done early if your intention is to do it only so that no one will notice a change in your appearance. If the results are too subtle, the surgery probably wasn’t necessary in the first place.
Modern hair restoration surgery, properly performed, will be virtually undetectable after a week to ten days, and grows in slowly over the course of a year. Therefore, doing a hair transplant early, so that the existing hair will camouflage the procedure, is also unnecessary and not a good reason to have surgery. Have the procedure when you are unhappy with the amount of hair you currently have.
Diagnosing Hereditary Hair Loss in Men
The diagnosis of androgenetic alopecia in men is made by observing:
- a “patterned” distribution of hair loss (see Norwood classification below)
- the presence of miniaturized hair in the areas of thinning
- a normal, non-scarred scalp in the bald area
The diagnosis is supported by:
- a positive family history of androgenetic hair loss
- the elimination of other causes of hair loss (this is particularly important in diffuse alopecia where there is no specific pattern (see below)
As we have discussed, miniaturization is the progressive decrease of the hair shaft’s diameter and length in response to androgens, specifically DHT. It can best be observed using a densitometer, a hand-held instrument that magnifies a small area of the scalp where the hair has been clipped to about 1mm in length.
 Hair Densitometer
Hair Densitometer Hand-held Microscope
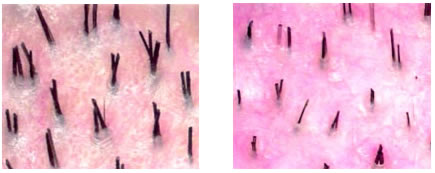
Hand-held MicroscopeThe photo, below left, was taken from a normal scalp. The follicular units (groups) are made of predominately thick, healthy terminal hair. Note the relatively uniform diameter of the hair shafts. The photo, below right, shows that many hairs have decreased in diameter (miniaturized). This is characteristic of androgenetic alopecia.
The diagnosis of androgenetic alopecia is supported by a family history of hair loss, although a positive history is not always identified. There is a slightly greater incidence of having a positive history on the mother’s side but, as we have mentioned before, the inheritance of male pattern hair loss can come from either side of the family.
If the hair loss is diffuse (thin all over the scalp) rather than following one of the specific Norwood patterns, the diagnosis can be more difficult. However, the presence of miniaturization in the areas of thinning usually confirms the diagnosis of androgenetic alopecia. If the diagnosis is still unclear, a number of other conditions must be ruled out.
Medical conditions that can produce diffuse hair loss include thyroid disease and anemia. Certain medications, including some drugs used for high blood pressure and depression, and the use of anabolic steroids, can also cause male hair loss.
The following laboratory tests are often useful when a non-androgenetic cause for diffuse hair loss is suspected: blood chemistries, complete blood count, serum iron, thyroid functions, and tests for lupus and syphilis.
When the diagnosis of androgenetic alopecia is still uncertain, further diagnostic information can be obtained from a hair-pull test, a scraping and culture for fungus, a microscopic examination of the hair bulb and shaft, and a scalp biopsy. A dermatologic consultation is warranted whenever the cause of hair loss is unclear.
Classification of Hair Loss
Once a diagnosis of androgenetic hair loss has been confirmed, you can compare your degree of baldness with the standard charts that follow. The Norwood classification, published in 1975 by Dr. O’tar Norwood, is the most widely used classification for hair loss in men. It defines two major patterns, the regular pattern and the Norwood Class A pattern. A third, common type of androgenetic hair loss, that of diffuse pattern and unpatterned alopecia, has been detailed by this author [Follicular Transplantation: Patient Evaluation and Surgical Planning. Dermatologic Surgery 1997]. The most common system used to describe the pattern of hair loss in women is the three stage classification proposed by Ludwig.
Regular Norwood Pattern
In the regular Norwood pattern, hair loss begins in two distinct areas, the temples and the crown. Over time, these areas enlarge and gradually coalesce until the entire front, top and crown (vertex) of the scalp are bald. [The area where the hair forms a swirl in the back of the scalp, the same area where hair often begins to thin at an early age, will be referred to as the crown or vertex. These terms will be used interchangeably throughout the text.] The regular Norwood pattern of hair loss is divided into seven stages. Since hair loss is continuous, many patients will fall into overlapping categories.
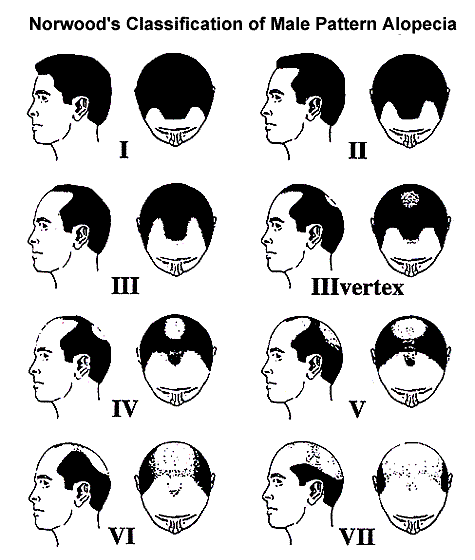
Norwood Class I represents a normal adolescent or juvenile hairline – it does not signify balding. The adolescent hairline generally rests on the upper brow crease (the highest wrinkle on the forehead) and has a horizontal or flat appearance. Class II indicates a progression to the adult or mature hairline. This position is approximately one finger’s breath (1.5cm) above the upper brow crease in the middle of the forehead, with some recession towards the temples. This also does not represent balding. Class III is the earliest stage of male pattern hair loss. It is characterized by a deepening temporal recession. When there is also some thinning in the crown, the pattern is called a Class III Vertex. Early Class III hair loss should be treated with medication rather than surgery, particularly in a younger person.
Norwood Class IV is characterized by further frontal hair loss and enlargement of the vertex, but there is still a solid band of hair across top of the scalp that separates the front and vertex. In Class V, the bald areas in the front and crown continue to enlarge and the bridge of hair separating the two areas starts to break down. A person is classified as a Class VI when the bridge of hair disappears forming a single, large bald area that extends from the front of the scalp into the crown. The hair on the sides of the scalp remains relatively high. In Class VII, the most advanced stage, only a wreath of hair remains in the back and sides of the scalp to produce a characteristic “horse shoe” pattern.
Norwood Class A
The Norwood Class A pattern is characterized by a front to back progression of hair loss. In Norwood Class A’s, there is one continuous area of balding. When the hair loss extends into the crown, the area of balding is generally more limited than in the regular Norwood classes. The Class A pattern is divided into five stages.
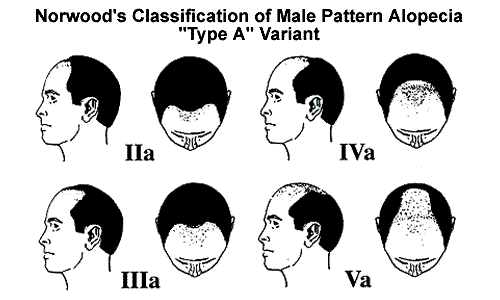
In a Norwood IIa, there is recession at the frontal hairline, particularly in the mid-portion. In a Norwood IIIa there is an extension of the hair loss further back with involvement across the entire frontal hairline. In a Class IVa patient the entire frontal area is bald. In a Class Va, the hair loss extends into the crown. At times a Norwood Class 5A will continue to bald and become a regular Class VI. It is very rare for a person with a Class A pattern to eventuate into a regular Norwood VII.
The Norwood Class A patterns are less common than the regular pattern (< 10%), but are significant because of the fact that, since the hair loss is most dramatic in the front, the patients look very bald even when the hair loss is minimal. Men with Class A hair loss often seek surgical hair restoration early, as the frontal bald area is less responsive to medication and the dense back and sides contrast and accentuate the baldness on top. Fortunately, Class A patients are excellent candidates for surgical hair restoration.
Diffuse Patterned and Unpatterned Alopecia
Diffuse Patterned Alopecia (DPA) is an androgenetic alopecia manifested as diffuse thinning in the front, top and crown, with a stable permanent zone. In DPA, the entire top of the scalp gradually miniaturizes (thins) without passing through the typical Norwood stages.
In Diffuse Unpatterned Alopecia (DUPA) the back and sides thin as well, so that there is no stable permanent zone. The hair loss in persons with DUPA tends to advance faster than DPA and more often ends up in a horseshoe pattern resembling the Norwood class VII. However, unlike the Norwood VII, the DUPA horseshoe can look almost transparent due to the low density of the back and sides.

Differentiating between DPA and DUPA is a fundamental part of the evaluation of hair loss, since those with DPA are often good candidates for hair transplantation, whereas DUPA patients almost never are, as they eventually have extensive hair loss without a stable zone for harvesting the donor hair.
Patients with DUPA often begin to thin in their teens. The early diagnosis of DUPA can be made with a densitometer by noting increased miniaturization in the donor area. Although these changes can be identified at a relatively early age, they can often be subtle and easily missed by the inexperienced physician. With time, the miniaturization becomes more obvious, so that by the age of 25, the identification of those patients who will eventuate in DUPA is relatively straightforward, even without densitometry. Insuring that the donor area is going to be stable over time, presents a compelling argument for not performing hair transplants on people that are too young.
Classification of Hereditary Hair Loss in Women
The Ludwig Classification uses three stages to describe female pattern genetic hair loss: Type I (mild), Type II (moderate) and Type III (extensive). In all three Ludwig stages, there is hair loss on the front and top of the scalp with relative preservation of the frontal hairline. The back and sides may or may not be involved.

Type I

Type II

Type III
In Ludwig Type I, there is early thinning that can be easily camouflaged with proper grooming. Type I patients have too little hair loss to consider surgical hair restoration.
Women with Type II hair loss have significant widening of the midline part and noticeably decreased volume. Hair transplantation may be indicated if the donor area in the back and sides of the scalp is stable.
In Ludwig Type III, there is a thin, see-through look to the top of the scalp. This is often associated with generalized thinning over the entire scalp. Often patients that have progressed to this stage have too little donor hair to make surgical hair restoration worthwhile.
All women experiencing hair loss should have an accurate diagnosis made, preferably by an experienced dermatologist. This is particularly important since the diffuse hair loss that women typically develop, can occasionally be caused by a number of treatable medical conditions. Regardless of the extent or cause of hair loss, only women with stable hair on the back and sides of the scalp are candidates for hair transplantation.
Continue reading this hair restoration book:
Chapter 5 – Psychology of Hair Loss »»
Table of Contents
| Introduction | |
| Chapter 1 | Brief History of Hair |
| Chapter 2 | Hair and Its Functions |
| Chapter 3 | Causes of Hair Loss |
| Chapter 4 | Hereditary Baldness |
| Chapter 5 | Psychology of Hair Loss |
| Chapter 6 | Hair Loss Medications |
| Chapter 7 | Hair Transplant Basics |
| Chapter 8 | Follicular Unit Transplantation |
| Chapter 9 | Follicular Unit Extraction |
| Chapter 10 | Master Plan for Restoring Hair |
| Chapter 11 | Goals and Expectations |
| Chapter 12 | Numbers of Grafts Needed |
| Chapter 13 | Hair Transplant Repair |
| Chapter 14 | Hair Loss in Women |
| Chapter 15 | Hair Systems and Camouflage |
| Chapter 16 | Preparing for a Hair Transplant |
| Chapter 17 | The Hair Restoration Procedure |
| Chapter 18 | What to Expect Following Surgery |
| Chapter 19 | Hair Transplant Fallacies |
| Chapter 20 | Choosing Your Doctor |
| A Final Note | |
| References | |
| About the Author |






