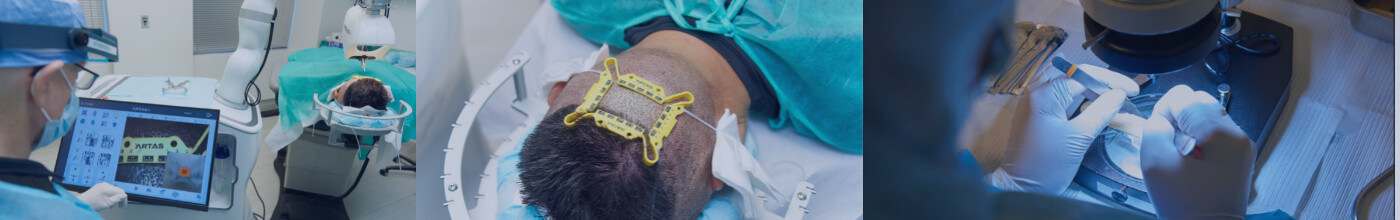
Robotic FUE is an advanced form of hair transplant that uses robotic precision to harvest and place follicular units with minimal trauma. At Bernstein Medical, we use the ARTAS® iX Robotic System to assist with the most complex parts of the Follicular Unit Extraction (FUE) procedure, follicular unit harvesting, and recipient site creation.
This robotic system uses advanced digital imaging and algorithms to enhance the accuracy and speed of each step. It’s a significant advancement over manual FUE, offering better consistency, less discomfort, and no linear scar.
Pioneered at Bernstein Medical
Bernstein Medical was among the first practices in the world to use robotic technology for hair transplantation. Dr. Bernstein and Dr. Rassman collaborated with Restoration Robotics to bring the ARTAS system into clinical practice. They developed many of the initial protocols that shaped robotic hair restoration as we know it today and continue to consult on software and hardware improvements.
We were the first to perform FUE using the ARTAS Robotic Hair Transplant System and the first to upgrade to the ARTAS iX. We are proud to be recognized as an ARTAS Clinical Center of Excellence, serving as a beta testing site for advancements in robotic hair transplant technology.
How the ARTAS Robot Works
The procedure begins with local anesthesia and placement of a skin tensioner, a device that stabilizes the scalp and optimizes access to the donor area. The robot then scans the area to identify individual follicular units for harvesting.
Using advanced AI, the ARTAS system evaluates the angle, depth, and density of each follicle in real time. It then uses a two-step, sharp–blunt punch technique to isolate grafts without damaging surrounding tissue. Once grafts are dissected, they’re removed manually by a trained technician.
When recipient sites are created, the physician programs the design into the robot based on the patient’s natural growth pattern. The robot then makes incisions according to that custom plan.The result is precise, natural-looking placement with uniform spacing, direction, and depth, far beyond what’s possible through manual techniques alone.
For a more in-depth review of how the robotic hair transplant system works, visit the page on ARTAS Robotics.
Advantages of Robotic FUE
Compared to traditional FUE, robotic harvesting offers greater speed and consistency. The ARTAS robot eliminates the variability caused by human fatigue or manual errors, particularly during extended sessions. This helps ensure uniform graft quality, shorter procedure time, and better healing.
Robotic site creation also protects existing hairs in thinning areas, allowing us to enhance density without compromising natural hair. It’s particularly beneficial in complex cases such as hairline refinement and crown restoration.
Graft Harvesting
In traditional FUE, surgeons manually align the punch tool with the direction of hair growth, which varies from follicle to follicle.
The ARTAS system automatically calculates these variables and adjusts its dissection path to match each follicle’s natural angle. This reduces transection rates and improves the survival of each graft.
Recipient Site Creation
Using a physician-defined pattern, the robot creates recipient sites with consistent spacing, direction, and angle, mimicking the patient’s native hair flow. The system can generate over 1,000 recipient sites per hour, making it far more efficient than manual site creation.
The physician programs the hairline design into the system, and the robot carries it out precisely, preserving aesthetics while protecting existing hair.
Benefits of Robotic FUE
- Minimally invasive procedure
- No scalpel, no stitches, no linear scar
- Quick recovery, minimal downtime
- High graft survival rate
- Natural-looking, permanent results
What sets Robotic FUE apart is its ability to deliver consistent results with minimal disruption to the surrounding scalp tissue. The system’s precision means less trauma, less bleeding, and a smoother healing process. By combining surgeon oversight with robotic execution, patients benefit from personalized care and the accuracy of advanced technology.
Ideal Candidates for Robotic FUE
Patients who are good candidates for Robotic FUE typically:
- Prefer to wear short hairstyles
- Want to avoid a linear scar
- Are in good general health
- Have sufficient donor hair in the back and sides of the scalp
- Are looking for a more comfortable and efficient procedure with predictable results
Robotic FUE is also ideal for patients who have already had a strip procedure and are looking to improve density without additional scarring.
What Makes the ARTAS iX Unique?
The ARTAS iX is the most advanced version of the ARTAS robot to date. It includes both follicular unit harvesting and site creation in one system—streamlining the procedure and improving precision throughout.
Features of the ARTAS iX include:
- Real-time 3D analysis and tracking
- Artificial intelligence that adjusts to subtle changes in scalp positioning
- A robotic arm that performs thousands of precise movements without fatigue
- A high-definition stereoscopic vision system
- Faster graft dissection and placement, reducing the overall time in surgery
Robotic Hair Transplants at Bernstein Medical
Bernstein Medical continues to lead in robotic hair transplant surgery by adopting the latest ARTAS system updates and refining robotic hair restoration techniques. Our experienced surgical team leverages the ARTAS robot’s capabilities to deliver consistently excellent results tailored to each patient’s unique hair characteristics and restoration goals.
Custom Punch Sizes for Personalized Results
Bernstein Medical was among the first to refine follicular unit extraction with individualized punch sizes tailored to each patient’s hair type and scalp characteristics. Instead of relying on the industry-standard 1.0mm punch, we use smaller options—like 0.8mm and 0.9mm—to minimize scarring, shorten healing time, and preserve more follicular units during harvesting. These smaller punches produce grafts with less surrounding tissue, simplifying placement and improving overall efficiency.
Some patients, especially African-Americans, have less transection with the larger punch, so selecting the appropriate tool for each patient is an important decision that the physician must make, as this can have a significant effect on the outcome of the transplant.
Discreet Coverage with Long-Hair Robotic FUE
Our long-hair technique allows patients to maintain coverage in the donor area immediately after surgery. By lifting and trimming a narrow band of hair at the back or sides of the scalp, we extract follicular units without shaving the entire area. Afterward, the longer surrounding hair is combed down to conceal the donor zone.
Long-hair robotic hair transplant procedures are generally performed through one long band or through two separate parallel bands above and below a linear donor scar. Corners are generally rounded and the edges are feathered using the ARTAS system so the harvested area blends in with the surrounding hair.
Smarter Harvesting with the Graft Selection Algorithm
Earlier versions of robotic FUE selected grafts at random, but our system now uses a graft selection algorithm to prioritize multi-hair follicular units. By skipping smaller grafts—like those with just one hair—we can increase the number of hairs harvested per session while reducing the number of incisions in the donor area.
When smaller units are needed, such as to create a natural-looking hairline, the robotic graft selection algorithm is placed on OFF. Alternatively, robotically-extracted units of three or more hairs can be dissected into smaller units by a technician.Our team’s extensive experience with stereo-microscopic dissection—gained through years of FUT procedures—allows us to reshape larger grafts into refined units that enhance the look of cosmetically sensitive areas.
Pre-Made Recipient Sites for Better Graft Survival
At Bernstein Medical, we often create recipient sites in advance—before harvesting even begins. This strategy ensures grafts are placed as soon as they’re ready, reducing time outside the body and boosting survival. Pre-making sites also improves visibility, minimizes bleeding, and accelerates healing.
The technique minimizes the time grafts are outside the body, increases visibility when placing the grafts (due to less bleeding), minimizes graft popping, and allows the recipient area to start the healing process earlier.
Advanced Techniques with the ARTAS Robot
From enhanced donor site blending to targeted graft harvesting, our approach goes beyond standard robotic extraction. Each technique is designed to improve precision, reduce scarring, and optimize aesthetic outcomes tailored to the individual.
Feathering
To ensure a seamless transition between the harvested area and the surrounding scalp, we use the ARTAS system to gradually taper the edges—a technique known as feathering. This is particularly important on the sides, where thinning hair may offer less natural coverage.
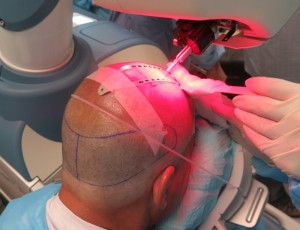
Focal Harvesting
Focal harvesting allows us to target untouched zones or supplement areas from a prior session. The ARTAS robot can focus on specific regions to increase yield without compromising the overall appearance of the donor area.
The lower area of the picture shows the Robot focusing on areas that had been missed in the previous FUE session.
Robotic FUE at Bernstein Medical
At Bernstein Medical, robotic hair restoration procedures are performed using the ARTAS system, combining advanced technology with expert clinical oversight. Each session is carefully planned to match your unique hair pattern, ensuring natural, lasting results.While the ARTAS robot handles graft harvesting and site creation with remarkable precision, your surgeon directs the overall plan, including graft placement and hairline design.
Our experienced medical team monitors every step of the process, so you benefit from both cutting-edge robotics and personalized care. Schedule your consultation today and take the first step toward a more confident you.
Frequently Asked Questions About Robotic FUE Hair Transplants
It typically takes 6 to 8 hours, depending on the number of grafts. Because the robot increases speed and precision, large sessions can be completed more efficiently than traditional FUE.
The procedure is performed under local anesthesia, so you shouldn’t feel any pain during the surgery. Most patients experience only mild soreness or swelling afterward, which subsides within a few days.
Robotic FUE leaves tiny, round scars that are nearly invisible, even with short haircuts. The results look completely natural.
While both techniques can produce excellent results, Robotic FUE offers greater precision, consistency, and speed—especially for patients requiring a large number of grafts or those concerned with minimizing scarring.
Most patients return to non-strenuous activities within 2-3 days. Any redness in the donor area typically fades within a week.
Feathering of the extraction zone in FUE is a technique where the distance between the extractions gradually increases as one reaches the border of the extracted zone. When this technique should be used depends upon the short- and long-term goals of the patient. If the patient’s main goal of the FUE procedure is to wear their hair very short, then the technique of feathering and rounding the edges to have a less distinct border is appropriate, as this will decrease the visibility of the harvested area.
However, if a person does not wear his hair very short (nor plans to) and maximizing the donor supply is paramount, then a more organized pattern, with less feathering, will give a greater long-term yield and a more even distribution. The reason is that the healing of FUE wounds distorts adjacent follicular units making subsequent extraction in the same regions more difficult and increases the risk of transection. For this reason, in subsequent procedures we generally prefer to harvest in new areas. If we need to harvest more hair from the same area, we rarely go back more than once.
When one feathers extensively in the donor area, this utilizes a larger surface area of the scalp with less graft yield, so it may become necessary to go back over the same area to obtain additional grafts, often multiple times. This risks increased transection and an uneven, mottled appearance to the donor area.
If a person wears his hair very short, then feathering is critical (even though it makes subsequent extraction more problematic). It is very easy to feather and round edges with the ARTAS robot, but we make the decision to do so based upon the specific needs and goals of the patient.
The ARTAS robot is a physician controlled, computerized device that uses a three-dimensional optical system to isolate follicular units from the back of the scalp in a hair transplant. The robotic system assists the physician in the extraction of grafts with precision and speed. Although there is some advantage to having “human feel” for the tissue, this is far outweighed by the fact that repetitive procedures performed manually thousands of times lead to operator fatigue and result in increased transection and damage to grafts. With the ARTAS robotic system, the quality of the first and the last graft harvested will be the same.
Read about advantages of the ARTAS Robot over manual FUE procedures
Restoration RoboticsOpens in new window has been very responsive to the needs of its physicians and to their patients. Because I work closely with Restoration Roboticsin the development of new improvement and advances they are often introduced first in our practice.
The ARTAS robotic system can be used in patients with any hair color although in order for the robot to visualize white hair (or very light blond hair) the hair must be dyed. Curly hair is also not a problem as the donor hair in a robotic procedure is shaved to approximately 1 mm in length so a wave or curl is eliminated. In patients of African descent, where the hair below the surface of the skin may be curved, a slightly larger punch can be used. we have patients dye their hair the evening before or the day of the procedure. For convenience, only the hair in the donor area (back and sides) where the robot will be doing the harvesting needs to be dyed.
In patients who prefer not to shave or dye the entire back and sides of the scalp, we can perform the ARTAS robotic FUE using the long-hair technique. With this technique, you will grow your hair on the back and sides of the scalp a bit longer so it can cover the harvested area. On the day of the procedure, we will lift up the hair, clip a long thin band of donor hair and then extract follicular units from this limited region of the scalp. After the procedure, you can simply comb down your hair to cover the donor zone. The area that has been harvested (and possibly dyed depending on your hair color) will not be visible.
With any type of hair transplant it takes 10 days for the transplanted grafts to be permanently fixed in place. The difference between FUE and FUT is in the limitations of activity due to the donor area. With FUE one would need to abstain from MMA for the same 10 days it takes the recipient area to heal (the grappling component of Mixed Martial Arts is the most stressful on the scalp). With FUT, however, one would need at least three months for the linear donor scar to heal before one could resume contact sports like MMA.
At the outset of the procedure, the physician sits at a computer terminal that is connected to the ARTAS Robot and enters the specifications directly into the robot’s software. Variables programmed in this manner include the number of recipient sites, density of sites, angle that the hair will extrude from the skin, depth of recipient sites, and the minimum distance away from existing hair follicles that a site can be created.
Robotic FUE may cost slightly more per graft than a typical manual FUE procedure due to the greater expense of this new technology. At Bernstein Medical, we use the ARTAS Robotic System for all Follicular Unit Extraction (FUE) procedures.
The ARTAS robot‘s optical guidance system enables it to accurately create recipient sites in areas of thinning hair without damaging existing hair follicles. During the recipient site creation process, the robot uses its advanced image-guided optical system to scan the surface of the skin, locate existing hair follicles in the recipient area, and then create recipient sites at a specified distance from these existing hairs.
The ARTAS robot carries out this process rapidly, accurately, and consistently according to the physician’s programmed specifications. Thanks to the microscopic precision of the image-guided technology, the robotic hair transplant system can avoid injury to follicles that can result when Follicular Unit Extraction (FUE) is performed using manual techniques.
The ARTAS® Robotic Hair Transplant system eliminates the inconsistencies inherent in creating large numbers of recipient sites by hand. The robot can create sites at a rate of up to 2,000 per hour. Although there is more set-up time compared to sites made manually, once the physician specifies the parameters such as punch depth, punch angle, and site direction, recipient site creation is precise and rapid.
One of the benefits of robotic site creation is that the distribution of grafts over a fixed area of the scalp can be exact. For example, if one wants to transplant 1,000 grafts evenly over 50cm2 of area, this can be done with great precision and with uniform site spacing. In addition, the physician can vary the densities in select regions of the scalp and the robot will adjust the densities in other areas so that the total number of sites remains the same.
Another benefit of the new technology is that the robot can be programmed to avoid existing hair and select which specific hair diameters to avoid. The robot is programmed to keep a specified distance from the existing hair to ensure that the resident follicles will not be damaged and that the distribution of new hair is even and natural. This computerized mechanism appears to be more accurate than what can be done by hand and, importantly, does not sacrifice speed in the process.
In performing recipient site creation, the ARTAS Robotic Hair Transplant system automates another part of the hair transplant process that is repetitive and prone to human error. In robotic site creation, the physician first designs the hair restoration and then specifies the angle of hair elevation, hair direction, site depth, average density, and total number of the recipient site incisions. The robot then creates the sites according to these specifications.
During site creation, the robot automatically uses its image-guided technology to avoid hairs of a certain diameter (specified by the doctor). The robot creates sites at a minimum distance from hairs of the specified diameter (the distance is also specified by the physician) and will do so randomly throughout the areas where the hair is finer or the scalp is bald. With this important feature, the new distribution of sites can be made to complement the distribution of existing hair. Observation of the ARTAS System suggests that it performs recipient site creation with greater precision and consistency than can be accomplished manually.
There are two basic types of hair transplant procedures, Follicular Unit Transplantation (FUT or strip surgery) and Follicular Unit Extraction (FUE).
In FUT, donor hair is harvested by removing a long thin strip from the back of the scalp. Individual follicular units are then obtained from this strip using stereo-microscopic dissection. In FUE, individual follicular units are harvested directly from the donor area using a sharp, round cutting instrument.
The ARTAS Robotic System performs the follicular unit isolation step of an FUE procedure and can also create recipient sites according to specifications determined by the hair restoration surgeon. In performing each of these steps, the robot uses its image-guided technology to locate the next target and position the cutting instrument, and it does so with precision and speed that cannot be accomplished using manual FUE techniques or instruments.
The ARTAS robot uses a dual operating system when performing follicular unit extraction. One station consists of a desktop computer adjacent to the robot. This station is used to establish the basic parameters of the transplant such as the spacing of grafts, the angle and depth of the harvest, which size follicular units will be targeted, and a host of other important variables.
The hand-held pendant is used by the operator situated next to the patient. The remote has more limited options – the main ones being depth adjustment and to immediately suspend the action of the robot. Many of the parameters are determined automatically by the robot’s computer to maximize the accuracy of the harvesting. The robot also makes real-time adjustments to these variables during the hair restoration procedure.
The physician sets the parameters at the computer monitor and, once the settings are determined, he/she sets the tensioner grid on the patient’s scalp. The tensioner determines where the grafts will be harvested. The grid is moved approximately every 130 harvests. The robot can be operated at the computer terminal and through a mobile pendant. The physician often alternates with a trained assistant between that station and using the pendant.
Besides the involvement in the operation of the robot, there are many other important physician-dependent steps to the hair transplant including the planning and design of the procedure, and recipient site creation. Other steps, such as the microscopic sorting and trimming of harvested follicular unit grafts and graft placement, are often performed by trained staff, but require the physician’s close supervision.
The ARTAS robotic system is equipped with advanced sensors that determine the precise depth of the sharp and blunt needles used both in the graft harvesting step and for recipient site creation. The robot automatically adjusts to the precise depth needed for the non-traumatic extraction of the grafts. The tip of the punching mechanism contains depth markings so that the physician can visually override the punch when he wants to fine-tune its action. While monitoring the procedure in real time, if it is observed that the punches are too superficial or too deep, punch depth can be modified using the robot’s computer system.
The physician can also use the ARTAS system to precisely control the depth of recipient sites. As with harvesting, the robot automatically adjusts the depth based on parameters set by the physician and the doctor can then make further adjustments, in real-time, during the procedure.
As with manual FUE, robotic FUE hair transplantation is an outpatient procedure performed under long-acting local anesthesia – a combination of lidocaine and bupivacaine. After the initial injections, the patient does not experience any pain or discomfort.
Before starting local anesthesia, we give most patients oral valium and intra-muscular midazolam (a very fast acting sedative that is very relaxing). While some patients doze off at the beginning of the procedure, others prefer to watch TV, a film, or just chat.
Local anesthesia generally wears off after 4-5 hours, so for transplant sessions lasting longer than this, we will give more anesthesia before the first wears off. With Robotic FUE, there is no discomfort once the procedure is completed and the anesthesia wears off. This is in stark contrast to an FUT strip procedure which can be uncomfortable in the donor area for days to weeks.
I performed a study (“Graft Anchoring in Hair Transplantation,” Dermatologic Surgery 2006; 32: 198-204) to answer a simple question, one that patients ask all the time: at what point are transplanted grafts so securely anchored in the scalp that they cannot be dislodged?
In the study, it was found that after 10 days the transplanted grafts become a permanent part of the body such that no amount of scrubbing or combing can dislodge them. So, while there are generally no limitations on strenuous exercise after a FUE procedure, we recommend waiting at least 10 days before playing any contact sport, like football, as the grafts could be dislodged if vigorously rubbed.
To learn more, see After Your Hair Transplant Surgery
We can extract the same number of follicles robotically as we can manually.
That said, the goal of any hair transplant procedure is not to transplant as many hair follicles as possible but rather to achieve the best possible cosmetic result given your degree of hair loss and the number of hair follicles available in your donor area.
While there is no difference between robotic and manual FUE in terms of the number of follicles that each procedure can extract, robotic FUE does have the following advantages over manual FUE:
- During the follicular unit extraction (or harvesting) phase of a hair transplant, there is less chance of damaging follicular units using a robot vs. a hand held device (e.g., Neograft), because the robot is more accurate. This means more grafts survive after transplant.
- Robotic graft harvesting times are shorter than manual, e.g., while on average if a physician could manually extract 200-300 grafts per hour, the same physician could robotically extract up to 500-1000 grafts per hour ((Chang, H.H. Robotics, artificial intelligence, and the future of hair transplantation. Prime Dermatology, July/August 2014.)). This means a shorter procedure time for the patient.
Read more about the advantages of Robotic FUE.
Although it is possible to have a hair transplant to the crown using robotic FUE in African American patients, given your young age and that you state your hair loss is progressing aggressively while on Propecia and Minoxidil, it is likely not a good decision to have surgery at this time.
The reason is that as your hair loss surrounding the crown expands over time, it may look unnatural to have hair transplanted solely to the crown region.
At your age, it is best to take Propecia (finasteride) and Rogaine (minoxidil), and if a transplant is indicated, to start at your frontal hairline and top of your scalp, the areas that will be most important cosmetically long-term.
In February 2014 we introduced new technology that allows the ARTAS Robotic System to assist the surgeon in recipient site creation. We are now using the ARTAS robot to make recipient sites in select hair transplant procedures. If designed and programmed properly by the doctor, robotic assisted recipient site creation can produce a hair transplant result that is as natural as when the surgeon does it by hand.
All hair transplant procedures, follicular unit transplantation (FUT) and follicular unit extraction (FUE), leave scars. FUT produces a linear scar at the back of the scalp that may be visible if you keep your hair short. FUE, on the other hand, leaves small dot scars at the back of the scalp that are not visible if you keep your hair short. These tiny scars will happen regardless of which FUE method is used, i.e., ARTAS robot, SAFE system, Neograft, or manual FUE. Some physicians who use the Neograft method advertise that there is no scarring involved when using the Neograft; however, this is not true: however, this is not true: there is some scarring associated with all FUE methods that increases with the total number of grafts harvested.
That is a great question and it gets to one of the key benefits of the robotic hair transplant system: its accuracy. When a surgeon is performing FUE using manual techniques, they must wear a headset that magnifies the scalp so they can see the follicular units more clearly than with the naked eye. The surgeon must visually and mentally process subtle nuances of the skin and follicular units for every one of the hundreds or thousands of units that are extracted. The ARTAS robot magnifies the surface of the skin in much the same way, but to a much greater extent. In addition, it is not subject to the limitations of the human eye, or human hand, and it is not subject to human error. The surgeon may not have exact hand-eye coordination. The surgeon may be concentrating on one aspect of the extraction, say following the angle of the hair, but might ignore another important aspect of the follicle, say its depth in the skin or its orientation. And, of course, the surgeon tires, both physically and mentally, from performing the hundreds or thousands of repetitive motions.
The robot’s image-guided system, on the other hand, does not experience these limitations. The robot magnifies the skin, detects each follicular unit and the nuances of the skin/hair characteristics, and then extracts that follicular unit with precision. When the imaging system detects changes to the skin, this new information is fed into the computer in real-time and the system adjusts automatically based on this feedback as it continues to harvest grafts. There is no distracting the robot, and the robot will not forget, or ignore, key variables in the extraction. The robot can extract thousands of follicular units without tiring from repetition or slowing down the extraction.
Based on my own practical experience using the robot, it is clear that the robot’s ability to estimate the position of the follicles under the skin and to extract it with precision is superior to manual techniques. Having used the ARTAS system for over three years, and having helped make improvements to the device since the first iteration, I have seen robotic technology substantially improve the outcome for my patients.
We can extract (and transplant) the same number of follicular unit grafts robotically as we can manually?
The goal of a hair transplant is not to simply transplant as many grafts as possible but to achieve the best possible cosmetic result given the number of hair follicles in your donor reserve. Remember, this is always a limited supply.
While there is no difference between robotic and manual FUE in terms of the number of follicular unit grafts that each can extract, robotic FUE does differ from manual FUE in several important ways.
First, there is generally less transection of the hair follicles with robotic FUE, since the method is more precise. This enables us to obtain follicular units with less trauma to the grafts.
Second, while the robot is not necessarily faster than the human surgeon, the robot is much more consistent since, unlike the human surgeon, it never fatigues and the accuracy is maintained throughout the entire procedure.
Read more about Robotic Hair Transplant
Currently, the ARTAS® Robotic System is a technology for extracting grafts. This is the most difficult part of a follicular unit extraction procedure, but it is only one part.
There are two other major parts to the FUE procedure: one part is the creation of recipient sites (in our practice, we create the recipient sites first, so that once we harvest the grafts, we can immediately place them into the scalp), and the other part is graft placement.
Recipient site creation involves more than merely making holes in the recipient area. It involves making decisions on hairline design, graft distribution, hair direction, recipient site size and depth. When done manually, the surgeon first designs the new hairline so that the hair transplant will look as natural as possible, particularly as the person ages. Next, the surgeon will demarcate the extent of the area to be transplanted and decide on the graft distribution (i.e., how much hair will be placed in each part of the scalp) and will then prepare a “recipient site” in the part of the scalp that has lost hair. The surgeon will then manually create incisions in the recipient site into which the follicular units will be placed.
On February 8, 2014, Dr. Bernstein unveiled “recipient site” creation capabilities of the hair transplant robot. These new capabilities allow the doctor to import a hairline design and other markings that have been made on the patient’s scalp directly into the robot. The robot then maps the design onto a precise 3-D model of the patient’s head. The physician can then program the proper distribution, direction and depth of the future recipient sites and the robot then creates the sites according to the physician’s specifications.
Graft placement, the last step, is perhaps the most challenging to automate. Engineers are currently working to design and build the capacity to automate the placement of extracted follicular units into recipient site incisions. Done manually, it requires significant hand-eye coordination and a very slow learning curve. For the hair transplant robot, it will be a significant challenge with development taking several years or more.
Read more about Robotic Hair Transplant
There is no difference in the rate of growth between manual FUE verses robotic FUE. However, with Robotic FUE, the actual growth should be better due to less transection, i.e., less damage to follicles during the harvest.
In general, one can expect transplanted hair to start to grow within two to five months with the transplanted hair taking on its final appearance after approximately one year.
Robotic FUE is a significant improvement over other FUE techniques for a number of reasons. The accuracy and ability of a robot to perform countless repetitive motions are key reasons why robotic techniques are an improvement over manual techniques.
In a manual procedure, the skill and speed of a physician are under constant stress, as he or she must follow the angle and depth of the hair precisely hundreds to thousands of times. This task is almost impossible for even the best surgeons to perform without risking harm to the integrity of the follicles. Entering the skin at the wrong angle risks transecting or cutting the follicles and may render them useless for transplantation. Making too shallow an incision can also damage follicles, as the important base of the follicle can become sheared off when it is subsequently extracted.
The robot is engineered to avoid these problems, and so the number of viable grafts that the robot extracts is increased. As a result, the likelihood of the success of the transplant is greater using the robotic system.
Read more about Robotic Hair Transplant
I currently create the recipient sites by hand using different size needles. They determine the angle, direction and distribution of the grafts, and these three variables determine the aesthetic aspects of the hair transplant.
However, I am working with Restoration Robotics to have the ARTAS System create recipient sites and we are currently beta-testing this technology. The robot can now make very precise recipient sites. The ability of the robot to mimic the art of the surgeon is in the works, and we expect it to be ready in the fall of 2014.
In this new robotic-assisted process, the surgeon designs the hairline and delineates the area to be transplanted directly on the patient’s scalp. The surgeon then photographs the patient’s scalp and feeds the photograph into the robot’s computer to create a digital 3-D image. The doctor, in order to have the robot mimic what he would do by hand, can then manipulate various parameters, such as hair angle, direction and density.
Read more about Recipient Site Creation in a Robotic Hair Transplant
Currently the robot is only used for harvesting grafts from the donor area. In FUE, the doctor punches out hundreds to thousands of individual follicular units from the back and sides of the scalp by hand using a small round instrument called a punch. The punch has to be held at exactly the right angle, with just the right pressure applied, stopped at a precise depth and, during this time, rotated (or spun mechanically) without changing the alignment.
As one can imagine, this exhaustingly tedious process can best be done using the precision of a robotic device.
In FUT, the harvesting is done by a surgeon using a scalpel to make a long incision in the back of the scalp. It only takes a few minutes. The harvested strip is removed and then placed under dissecting microscopes where the individual follicular units are isolated. This dissection, thus far, can only be done by hand. There is no robotic technology available to do this.
Harvesting the donor hair, of course, is only one part of a hair transplant. The other steps, recipient site creation (making the holes that the grafts are placed into) and actually placing the grafts into those sites are similar in both FUE and FUT.
It is anticipated that robotic site creation will be available in the fall of 2014 and robotic graft placement, the third and final step, about two years after that. At that time, the robot will be able to perform the entire FUE procedure and the last two parts of the FUT procedure.
Of course, the robot doesn’t do the surgery alone. The physician must input all the information regarding the design and planning of the procedure and closely monitor each step of the robotic process. Unlike automating industrial production, the human scalp has great variability, so there is no one formula that will be appropriate for every patient. Physician skill and involvement is just as important in robotic hair transplantation as it is with every other type of surgical hair restoration procedure.
Great question. You are not giving me quite enough information to answer your question specifically, so I will answer in more general terms. If your donor hair supply was not good enough to do FUT (i.e. you have too little donor hair and too much bald area to cover) then most likely you will not be a candidate for FUE either, since both procedures require, and use up, donor hair. That said, if don’t need that much donor hair, but the nature of your donor area is such that a linear FUT scar might be visible then FUE might be useful.
An example would be the case in which a person has limited hair loss in the front of his scalp, has relatively low donor density, and wants to keep his hair on the short sides. In this case, FUT would not be appropriate as you might see the line scar, but we might be able to harvest enough hair through FUE to make the procedure cosmetically worthwhile. Remember, with low density neither procedure will yield that much hair to be used in the recipient area.
Another example is an Asian whose hair emerges perpendicular from the scalp so that a line incision is difficult to hide, i.e. the hair will not lie naturally over it. A third example is where the patient’s scalp is very tight. In this case, the donor density might be adequate, but it would just be hard to access it using a strip FUT procedure. In this case, FUE would also be appropriate.
From these situations, one can see that the decision to perform FUE vs FUT, or even a hair transplant at all, can be quite nuanced and requires a careful evaluation by a hair restoration surgeon with expertise in both procedures.
The ARTAS Robotic System, developed by Restoration Robotics, is the most advanced technology for extracting grafts (the first and most difficult step in a Follicular Unit Extraction procedure), but it cannot yet do the entire hair transplant procedure, nor can it work without the supervision of the hair restoration surgeon.
Currently, the ARTAS System assists the surgeon in performing the first part of an FUE hair transplant (i.e., the extraction phase) with greater precision and consistency than can be done by hand. Engineers and researchers are currently developing the ARTAS to do the remainder of the procedure as well, i.e., making recipient sites in parts of the scalp that have lost hair and then implanting the harvested grafts into these sites.
The next step, recipient site creation, will be available in the latter half of 2014. Dr. Bernstein is already testing a beta version of this new technology. We anticipate that within two years, under the supervision of the surgeon, the ARTAS robot will be performing most of the FUE hair transplant procedure.
When performing robotic hair transplants on patients with prior surgery, I program the robot to avoid scarred areas – just as we would do visually when performing manual FUE.
Your concerns are correct and would apply to any hair transplant procedure; FUT or FUE. That is why it is best not to begin hair restoration surgery too early.
I advise FUT because the grafts are of better quality (less transaction and more support tissue surrounding the follicle) and because more hair can be obtained from the mid-portion of the permanent zone –- which is where the hair is the best quality and most permanent. For the majority of patients a linear scar buried in the donor hair is not an issue. Each patient has to weigh the pros and cons of each procedure when making a decision.
I think that both procedures are excellent, which is why I do them both. My recommendations are determined by the individual patient. His or her age, desire to wear hair cut very short, athletic activities, donor density and miniaturization, extent of hair loss, and potential future balding are all important aspects in the decision process.
Cosmetically, the recovery for FUT is actually shorter, since the back and sides do not need to be shaved and the longer hair can completely cover the donor incision immediately after the Follicular Unit Transplant procedure. In large Follicular Unit Extraction procedures, the entire back and sides of the scalp need to be clipped very close to the scalp. It can take up to 2 or 3 weeks for the hair to grow long enough to completely camouflage the harvested area. Once the healing is complete and any redness has subsided, the hair can be cut shorter.
For strenuous physical activity, however, the recovery is longer with FUT due to the linear incision. This is a major reason why professional athletes or very physically active people prefer FUE. However, many business professionals prefer FUT hair transplantation as there is significantly less down time from work (for the cosmetic reasons discussed above).
Yes, the ARTAS robot for FUE can be adapted for African-American hair when performing follicular unit extraction. We use a punch that is 0.1mm wider in diameter than the instrument used for Caucasians. It allows us to incorporate the slightly larger volume of tissue that results from the curved hair and enables us to accomplish the hair transplant with less in jury to follicles than if a smaller instrument were used.
See before & after hair transplant photos of patients with curly hair
The ARTAS Robot performs follicular unit extraction just as well with blond hair as dark hair, but not white hair. It is simple to just to dye the white donor hair prior to the hair transplant procedure. This donor hair will be clipped very short the morning of surgery removed anyway, so it will not present too much of a cosmetic issue.
See before & after hair transplant photos organized by hair character
The recipient area is visible after both procedures for up to 10 days. The donor area in FUT is generally not visible immediately after the procedure. In FUE, the donor area must be shaved, so that will be visible for up to two weeks (the time it takes for the hair to grow in).
Thanks for your kind words. No hesitancy whatsoever. We find no increased risk. Think of it as if you did a hair transplant and ran out of grafts. The remaining sites don’t get infected, they just close up. In the process, all those chemotactic factors involved in the healing process move toward the wounds, so if a graft is placed into them, they would be less likely to get infected than a graft placed into a fresh (non-primed) wound, not more. It is like applying the surgical dressing Duoderm to a wound that helps it auto-sterilize. Putting the speculative science aside, we have not seen one single issue with it. Give it a try with an FUE or FUT procedure. Make the sites, have the patient takes his normal shower that night and you will be pleasantly surprised how little bleeding there is the next day and how easy it is to place the grafts.
Read a summary of the article on pre-making recipient sites
Read the full article as it was published in the Hair Transplant Forum International
Both FUT and FUE produce donor scarring; FUT, in the form of a line and FUE in the shape of small, round dots. With FUT hair transplantation, the line is placed in the mid-portion of the permanent zone, whereas in FUE the dots are scattered all over the donor area.
If a patient becomes extensively bald (i.e. the donor fringe becomes very narrow), the line of FUT will generally still remain hidden, whereas the dots of FUE will be seen above the fringe of hair. In the less likely scenario of the donor hair actually thinning significantly, both the line (of FUT) and the dots (of FUE) may become visible.
FUT (via strip) will give the best cosmetic results (more volume) since the grafts are of better quality (when using microscopic dissection, there is less transection and more surrounding tissue to protect the grafts) and better graft selection (the grafts can all be harvested from the mid-portion of the permanent zone).
In contrast, in FUE you need approximately 5 times the area. Because of this large donor area requirement, some of the hair must be harvested from fringe areas and thus the hair will be less stable genetically.
With subsequent FUT procedures we remove the first scar, so the patient only has one scar (albeit long). With subsequent FUE sessions we are adding additional scars, so over the long-term the cumulative scarring over large areas can present its own problems of visibility.
The main advantage of FUE is to have the option of wearing your hair very short (but not shaved). FUE is also appropriate for patients who are at risk for a widened donor scar (i.e., very athletic and muscular or with thin, tight scalps, etc.).
In my experience, Robotic Hair Transplantation is superior to other FUE methods in that it is much more accurate and more consistent. It enables the doctor to extract grafts with less damage than with hand-held instruments or other automated devices.
Correct, robotic FUE doesn’t work well on light-blond or white hair -– but it is easy to dye the hair prior to surgery, and this will solve the problem. We generally advise patients to dye their hair two to three days prior to the procedure so that any residue of the dying still on the scalp can be washed off.
The ARTAS robotic system, used at Bernstein Medical, has robotic control, video imaging and uses a blunt dissection technique. This allows for very precise extraction of follicular units from the donor area with minimal transection. The Neograft machine for FUE is a manually operated machine which uses sharp edge dissection. Because it relies on manual controls rather than robotics, it is less accurate and the cutting tip causes more graft injury. The precision of the robot allows the grafts to be harvested with less trauma and will thus result in better growth. In my opinion, these differences are very significant.
Read more about the differences between the ARTAS Robot and Neograft
In our practice, we charge the same per graft for both procedures. However, there is a slightly higher minimum fee for robotic FUE procedures. See our Hair Transplant Costs & Consultation Fees page.
The ARTAS robot only performs a small part of the FUE procedure, although it is an important one. FUE comprises four basic steps:
- Isolation of follicular units from the surrounding skin
- Removal of follicular units from the scalp
- Making recipient sites
- Placing grafts into these sites
The robot only performs the first step, follicular unit isolation.
Even in this first step, however, physician control is extremely important, as the doctor must determine the precise depth to which both the sharp and blunt dissection are set. They must also make constant adjustments to the angle that aligns the instrument with the graft.
The ARTAS robotic system gets all of its cues from the surface of the skin, so that it can place the target follicular unit in the exact center of the cutting field of the robotic tip. It can also align the tip parallel with the emergent hairs. However, the angle of the hair as it emerges from the scalp is slightly different than the angle below the skin and the doctor needs to tell the robot what this angle is. Fortunately, the robotic imaging system provides the doctor with the information he needs to make this determination.
Read about Robotic Hair Transplantation.
Yes. Although, the speed of removal per graft is about the same, the actual procedure time is shortened when using the robotic device. The ARTAS robotic FUE system has a longer set-up time, but this is more than offset by the fact that the robot doesn’t “tire” during longer procedures.
For more information, visit the page on Robotic FUE Hair Transplantation or read answers to questions on Robotic FUE.
There is only one, the robot called the ARTAS System for FUE, made by Restoration Robotics. The Neograft machine, occasionally confused with a robotic device, is actually a hand-held instrument that is not robotically controlled and lacks image-based tracking. It is, therefore, not capable of eliminating the operator error and variability of hand operated devices and does not decrease the damage to follicles, called transection, inherent in manual techniques.
Read more about Robotic FUE hair transplantation.
Robotic FUE leaves the same tiny, white scars in the donor area produced by manual Follicular Unit Extraction.
The Neograft device is basically a powered FUE tool. It is still done by hand and therefore risks operator induced errors and damage to hair follicles. The ARTAS System, made by Restoration Robotics, uses electronic image-based tracking capabilities to map the individual follicular units. It does so to determine the optimal approach for automated graft harvesting. The robotic harvesting device produces consistently high quality grafts and low dissection rates.
For more information on these systems, visit the Follicular Unit Extraction (FUE) section or read Dr. Bernstein’s answers to questions on Robotics.
The ARTAS System is a computer-guided method of harvesting follicular units in the donor area during Follicular Unit Extraction (FUE). The initial phase of FUE, where the follicles are selected, scored and separated from the surrounding scalp is done by the ARTAS System. All other phases of the procedure including; actual follicular unit graft removal from the scalp, hairline design, recipient site creation and placement of the grafts into the balding scalp are done by the surgical team.
In the near future, improvements in the ARTAS System should allow it to be able to actually extract the separated grafts from the scalp. Eventually, the engineers hope to be able to increase the capability of the system so that it can create recipient sites and implant the extracted grafts into them.
The ARTAS System for Follicular Unit Extraction (FUE) combines several features including an interactive, image-guided robotic arm, special imaging technologies, small skin punches of two different sizes, and a computer monitor. After the system is positioned over the patient’s donor area of the scalp, ARTAS is capable of identifying and isolating follicular units from the surrounding scalp.
After the robotic arm is aligned with the follicular unit, a sharp 1-mm punch is used to cut through the upper part of the skin (the epidermis and upper dermis).
Immediately following this, a duller, 1.3mm punch is used to separate the deeper part of the follicular unit from the remainder of the dermis and subcutaneous fat. Once separated by the robot, the follicular units are manually removed from the scalp and stored until they are implanted into the patient’s recipient area.
The ARTAS robotic system for hair restoration is a computer assisted system, made by a company called Restoration Robotics, that utilizes image-guided robotics to increase the quality of the hair follicles harvested during FUE. It aids in the initial part of the FUE hair transplant procedure where follicular units are separated from the surrounding tissue. The system is operated under direct physician supervision.
Restoration Robotics’ ARTAS System for robotic follicular unit harvesting, received 510K clearance by the Food and Drug Administration (FDA) on April 14, 2011. The indication is for “harvesting hair follicles from the scalp in men diagnosed with androgenetic alopecia (male pattern hair loss) with black or brown straight hair.”
Restoration Robotics is a medical device company, based in Mountain View, California, that has developed a computerized instrument to assist in the graft extraction phase of follicular unit extraction (FUE) hair transplant procedures. Their patented device, called “ARTAS,” is an image-guided system for FUE. Their website is: www.restorationrobotics.comOpens in new window.
Restoration Robotics, Inc. — based in Mountain View, CA — has spent the last few years developing and testing a robotic hair transplant device for follicular unit extraction (FUE). The ARTAS™ robot system has recently received 510(k) approval from the Food and Drug Administration, meaning that the company may now begin marketing the system for use in hair restoration clinics.
The FDA classifies the device as a “computer assisted hair harvesting system” and describes it as being used to identify and extract follicular units and to help the surgeon do the same during hair transplantation.
The ARTAS™ robot consists of a computer assisted station with needle mechanism, force sensor, robotic arm, and video imaging system. The software that runs the instrument helps the surgeon target follicular units for extraction and also uses stereoscopic video images to guide the needle mechanism and robotic arm.
We will update you as more information becomes available about the ARTAS™ system and Restoration Robotics.
See a photo of the ARTAS robot and stay on top of developments by visiting our Robotic Hair Transplantation page
Follicular Unit Extraction (FUE) using the Neograft machine is not painless and, while it does not produce a linear scar, it is surgery and there is significant scarring in the form of thousands of tiny holes that heal with round white marks.
In the video, Dr. Anthony Youn asks: “Do you wanna take a feel? It’s just a vacuum.” Rachel Ray states: “You don’t feel a thing.” Youn replies: “No [you don’t].”
This is very deceptive on the part of the doctor, since the instrument is basically a cutting instrument with the suction being used to remove and insert the grafts. Although the suction part would not be painful, the cutting part certainly is and requires the same anesthesia as a traditional hair transplant.
Our main concern is that the machine produces grafts that are sub-optimal with respect to quality and potential growth, as the Neograft’s suction apparatus tends to strip follicles away from their surrounding protective tissue and tends to dry the grafts out.
For in-depth information on this topic, read our pages on Follicular Unit Extraction (FUE) and the Neograft Machine for FUE.
If a follicular unit transplant is performed properly (using either extraction or a strip) there should be no bumps or surface irregularities. When the hair restoration is totally healed, the recipient area should be appear as normal looking skin.
With FUE it is important to sort out the grafts under a microscope, to make sure that all of the grafts placed at the hairline are 1-hair grafts and that the larger grafts are place behind the hairline. They should not be planted without first being sorted under a microscope.
I perform FOX tests on all patients when I am considering a FUE hair transplant. I do not routinely perform FOX tests before repairs (or on eyebrow transplants) where the number of grafts is relatively small.
The purpose of FUE is to identify those patients in whom FUE is inefficient — i.e. there is a greater than average risk of damage during the harvest. If this is the case, I would not perform the hair transplant since even slight inefficiencies create a significant problem when thousands of grafts are transplanted.
Remember, compared to Follicular Unit Transplant (FUT), FUE is a relatively inefficient procedure. Even when a small FUE hair transplant is performed (i.e., in a Norwood Class 3) we have to anticipate that eventually the person will need a large amount of grafts, so a FOX test is still important.
However, when the total number of grafts is small, such as in scar revisions or eyebrow restoration, small inefficiencies are not as important.
In addition, with repairs, the donor area is altered so that extraction in different areas may be very be different, rendering a FOX test in scar revisions far less useful.
Finally, if a FUE hair transplant is started, but then aborted due to extraction difficulties, the patient must either be reverted to a strip (which was not the preferred means of harvesting or a FUT would have been planned to begin with) or the patient will be left with a partial procedure – both less than ideal situations. However, if a FUE repair has to be aborted due to the inability to efficiently harvest hair, no harm was done; we just won’t be able to achieve our goal.
You can have shedding in the donor area from an FUE procedure, although it is not common. In FUE, the hair must be taken from the permanent zone and if there is too much wastage in the extraction process, too large an area may be needed to obtain the hair. This can leave a thin look even without shock loss (shedding).
Please see the Bernstein Medical – Center for Hair Restoration website as it explains Follicular Unit Transplantation (FUT) and Follicular Unit Extraction (FUE) in detail.
In brief, with FUT, follicular units are obtained from the microscopic dissection of a donor strip that has been removed from the back of the scalp. In FUE, the doctor attempts to remove intact follicular units directly from the scalp via a small round instrument called a punch.
Ultra Refined FUHT (Follicular Unit Hair Transplantation) is term that Pat Hennessey uses on his Hair Transplant Network. It refers to using very tiny recipient sites, carefully dissected follicular unit grafts, and large hair transplant sessions in FUHT procedures.
These are all terms that refer to the types of injury that can occur to grafts during a follicular unit extraction procedure.
In FUE, a sharp instrument (or sharp instrument followed by a blunt one) is used to separate follicular units from the surrounding donor tissue. Forceps are then used to remove the follicular units from the scalp.
Topping occurs in the first step when the doctor accidentally cuts off the top of the graft so that the remainder of the graft cannot be removed.
Capping occurs when the doctor grabs a graft with forceps and the top of the graft (the epidermis and upper dermis) pulls off, leaving the rest of the graft behind.
Tethering occurs when the bottom of the graft is still attached to the deeper tissues after the first step causing the follicular unit to pull apart during extraction.
There are a few other terms used as well.
Shredding occurs when the follicular unit is not totally separated from the surrounding tissue and pulls apart upon extraction. Shredding can also occur when the follicular unit was partially damaged in the first step.
Transection is like topping, but here the mid or lower portion of the hairs in the unit are cut.
Buried grafts occur when the graft is pushed into the sub-cutaneous space rather than extracted. Buried grafts can usually be removed, but if not removed completely, may turn form small cysts.
Visit the Follicular Unit Extraction page.
One of the causes of having pimples and redness following Follicular Unit Extraction may be buried hair fragments and there are significantly more hair fragments generated with the two-step FUE technique than with the three-step method.
In the three-step procedure, we use blunt dissection which minimizes transection (cutting of hair follicles) and thus reduces the incidence of hair fragments. See the Three-Step FUE page at the Bernstein Medical – Center for Hair Restoration website.
In our practice, we also place every extracted graft under the microscope. This serves a number of purposes:
- It gives me immediate feedback on transection rates, so that I can adjust my technique in real-time (using a stereo-microscope is much better than visual inspection for this purpose)
- It enables us to trim away excess tissue and hair fragments (we use the same judgment as we do with strip harvesting, so that a “viable looking” fragment would be left attached
- It allows us to accurately count the number of hairs in each follicular unit graft, as it is particularly important to have pure 1-hair grafts for the frontal hairline. This also allows us to better anticipate the end cosmetic result.
- It allows us to dissect larger follicular units into smaller ones for specific cosmetic purposes, i.e. eyebrows, hairlines, temples etc.
One of the ironies of FUE is that it is more efficient to extract the larger FUEs, since this gives us a greater hairs/hole ratio, but this often leaves us with an inadequate number of 1-hair units, which must be obtained though traditional stereo-microscopic dissection of the larger extracted grafts.
Other causes of folliculitis (manifested by pimples and redness) can result from placing the grafts too deep in the recipient site (where they may get buried) and secondary infection. A mild, transient folliculitis is often seen after a hair transplant without any precipitation factors.
In general, after a scar correction with follicular unit extraction you can clip your hair very short, but not shave your head. If you shaved your hair completely bald, you would generally see a vague outline of the linear scar as well as the small scars from FUE.
In general, FUT will give you more hair since, in FUT, the best hair from the mid-portion of the permanent zone of the scalp (also called the “sweet spot”) can be utilized in the hair transplant.
With FUE, since only the hair follicles are extracted and not the surrounding bald skin, if too much hair is removed, the donor area will begin to look thin as hair is removed. This will limit the amount of hair that can be harvested.
Although in FUE additional areas of the scalp can be utilized to some degree, this will generally not compensate for the inability to access all of the hair in the mid-permanent zone and the total amount available for the hair restoration will be less.
In follicular unit extraction, the area that is extracted is clipped to about 1-mm in length. However, if the session is not too large, then the clipped area can be long and thin so that the patient’s existing hair will cover it. The person’s hair should be left long for the procedure.
The first paper on Follicular Unit Hair Transplantation was published by Dr. Bernstein and Rassman in 1995 in the International Journal of Aesthetic and Restorative Surgery. The title of the paper used the abbreviated name Follicular Transplantation. The longer name “Follicular Unit Transplantation” was formalized by Bernstein et. al. in the paper “Standardizing the classification and description of follicular unit transplantation and mini-micrografting techniques.” This paper appeared in Dermatologic Surgery in 1998.
Follicular Unit Extraction derived its name from Rassman and Bernstein’s publication “Follicular Unit Extraction: Minimally invasive surgery for hair transplantation” that appeared in Dermatologic Surgery in 2002.
Although there is no line scar in follicular unit extraction, there are tiny round ones. You can clip your hair very short after FUE, however, shaving your head will make the very fine white scarring visible.
Follicular Unit Hair Transplantation, called FUT for short, is a procedure where hair is transplanted in the naturally occurring groups of one to four hair follicles. These individual groups of hair, or units, are dissected from a single donor strip using a stereo-microscope. The area where the donor strip was removed is sutured closed, generally leaving a thin, fine, line scar.
In Follicular Unit Extraction, or FUE, the individual units are removed directly from the back or sides of the scalp through a small round instrument called a punch. There is no linear scar. There is, however, scarring from the removal of each follicle. Although the scars of FUE are tiny and round, the total amount of scarring is actually more than in FUT.
In addition, since in FUE the bald skin around each follicular unit is not removed, the total amount of hair that can be removed in FUE is substantially less than in FUT. This is because if one were to remove all the hair in an area, it would be bald. In FUT, the intervening bald tissue is removed along with the follicles in the strip.
The combination of Follicular Unit Transplantation (FUT) and Follicular Unit Extraction (FUE) used the way you are suggesting does make sense and is actually how I originally envisioned the two procedures to work together.
The camouflage of the donor scar will probably never be necessary, but if it is desired, it should be postponed until after the last FUT procedure. FUE will make it possible for most people to wear their hair very short.
Read about FUT Hair Transplants
Read about FUE Hair Transplants
It is possible to use beard hair for a hair transplant, but there are three main differences between harvesting from the donor area and harvesting from the beard that should be taken into account. These are: 1) scarring 2) ease of extraction and 3) hair quality. Let’s explore these differences in turn.
First, in FUE, although there is no linear scar, there are small white round scars from where the hair is harvested. Normally these marks are hidden in the donor area and are not visible, even if the hair is clipped very short. However, if the scalp is shaven, these marks will become visible. When the beard is used as the donor source for the hair transplant, the patient must continue to wear a beard after the restoration, even if it is tightly cropped, or the faint white marks will show. The tiny round scars from FUE will generally be visible on a clean shaven face. As each person heals differently, we would perform a test before doing the actual procedure to make sure the marks from the extraction are not noticeable at the length that the person wants to wear his beard.
Second, FUE performed on beard hair differs from extraction from the scalp because of the greater laxity — or looseness — of facial skin. This makes extraction with minimal transection more difficult in some cases. A test prior to the hair transplant is particularly important in beard FUE so that the ease of extraction may be determined in advance.
Third, beard hair is coarser than scalp hair. Although the hair seems to take on some of the characteristics of the original hair in the transplanted area, the transformation is not complete. This makes beard hair an imperfect substitute for scalp hair.
A solution to the problem is to transplant beard hair behind the hairline for volume and scalp donor hair at the hairline for naturalness.
No. If hair was taken from outside the permanent zone as the surrounding hair continued to bald, the scars from FUE, although small, would become visible.
In addition, the transplanted hair would not be permanent, and over time would eventually fall out.
A robotic hair transplant is a type of hair restoration procedure where donor hair is removed directly from the back and sides of the scalp using robotic control. The specific type of hair transplant where robotic technology is used is called Follicular Unit Extraction (FUE). In FUE, a small round punch instrument separates individual follicular units (naturally occurring groups of 1-4 hairs) from the surrounding tissue so they can be extracted then implanted in the balding area. This process is very tedious and exacting, and when it is performed using manual instruments it often leads to significant damage or injury to the follicles.
Robotic technology allows the FUE procedure to be performed in a more precise and consistent way, ultimately maximizing the growth of the grafts. In a robotic FUE hair transplant, follicular units are extracted one at a time by the image-guided, computer-driven system called the ARTAS Robotic System, a technology developed by the company Restoration Robotics. At Bernstein Medical, all FUE procedures employ the speed and precision of the robotic system.
The indications for Robotic FUE are similar to manual FUE. FUE can be performed on any patient who is a candidate for a hair transplant. In general, robotic follicular unit extraction is particularly suited to patients who wish to maintain a short hairstyle and who are very physically active and want to return to sports or rigorous activity as soon as possible. FUE is also the treatment of choice for patients with very tight scalps or who have an increased risk of donor scarring.
As with manual FUE transplants, the ideal robotic FUE patient is one with stiff, coarse hair that is more perpendicular to the scalp (rather than lying flat) and whose skin possesses a thick dermis. These features are particularly striking in patients of Asian descent. Clinically, the robotic system is widely used on various hair types such as coarse straight hair, curly hair, and wavy hair of different colors. Robotic FUE is also very useful in African-American patients who are at risk to a having thickened donor scar from an FUT-strip procedure.
To determine if you are a candidate for Robotic FUE, you must have a hair loss consultation with a board-certified hair restoration physician.
The ARTAS System is composed of a robotic arm, dual-needle punch mechanism, video imaging system, and computer user interface. The double-punch arrangement consists of an inner (sharp) punch and outer (dull) punch.
The patient sits in a specially designed chair with their head down on a padded pillow. In this position, the robotic arm can access the donor area of the scalp. A grid-like device called a tensioner is applied to the donor area of the patient’s scalp. The tensioner has small dots called fiducials on its outer border which the robot “reads” for proper orientation. Using ARTAS iX, the robot automatically advances the robotic arm into position where the optical system analyzes the fiducials. The robot then uses the dual punch to isolate follicular unit grafts within the grid. The inner punch first scores the uppermost part of the skin, then the outer punch dissects the follicular units from the surrounding tissue, with the blunt edge helping to minimize injury to the grafts.
Once the system has made incisions around a hundred or more follicular units, special forceps are used to extract the units from the scalp and place them in a special holding solution. This process is repeated until the prescribed number of follicular units to be transplanted has been extracted from the donor area. The follicular units are then implanted manually into recipient sites created in the balding area and the transplant is complete.
Read details about how the robot works on the ARTAS Robotics page.
The length of your hair transplant procedure will depend upon how many follicular unit grafts are transplanted. Small to medium size sessions (fewer than 2,000 grafts) generally take one day. Larger FUE sessions will be performed over two consecutive days.
Recovering from a Follicular Unit Extraction hair transplant with the robot is the same as recovery with a manual FUE device. However, there is a significant difference between FUE and FUT procedures. Compared to FUT strip surgery, the donor area heals faster and with less discomfort after Robotic FUE. Also, with FUE there are no limitations on strenuous exercise after the procedure. After Robotic FUE you can resume your normal routine after one or two days.
While robotic and manual FUE procedures and FUT strip surgery will scar the donor area, the nature of the scarring is quite different: FUT leaves a linear scar, while FUE leaves many tiny white dots. Because of this, you will be able to wear your hair shorter after an FUE procedure than after FUT. Healing in the recipient area, where the grafts are placed, is the same in Robotic FUE, manual FUE, and FUT.
As with all Follicular Unit Extraction (FUE) procedures, the ARTAS robotic system is a minimally invasive hair transplant technique that does not require stitches or surgical staples. Instead of the sutured donor incision of a strip FUT procedure, robotic FUE leaves tiny round incisions that heal with little white marks that are imperceptible even with short hair.
The ARTAS robot is able to perform on dark hair, blonde hair, gray hair, very curly hair. With ethnic hair we use a 1.0mm punch instead of a 0.9mm punch. People who have white hair need to dye their hair before the Robotic FUE procedure in order for the robot to best visualize the hair follicles.
In robotic FUE hair transplant procedures, individual follicular units are harvested directly from the donor area using a sharp inner needle and an outer dull punch. The inner needle creates a shallow scoring incision that pierces the epidermis. The outer dull rotating punch dilates the scoring incision, dissects deeper into the scalp and frees up the follicular unit graft from the surrounding tissue. The robotic system uses a sophisticated optical system and algorithms to automatically detect hair on the scalp, target multi-hair follicular units, calculate the appropriate angle of dissection and adjust the depth of dissections based on physician inputs. A suction system lifts the graft up above the scalp, facilitating manual forceps extraction of the grafts. The robotic FUE system has the advantages of precision that does not fade over thousands of harvests and the ability for the physician to override the system when needed. The peer-reviewed literature states that transection rates of the robotic FUE technique are between 4.9%-6.6%. ((Shin JW et. al. Characteristics of robotically harvested hair follicles in Koreans. JAAD 2015; (72)1:146–150.)), ((Avram M, Watkins S. Robotic follicular unit extraction in hair transplantation. Dermatol Surg 2014; 40:1319–1327))
Graft selection is the key to obtaining the most hair with the least amount of donor area wounding. In the robotic system, the physician programs the robot to select grafts based on the desired hair content and establishes the field from which those grafts are harvested. The visual field is converted to an enlarged digital image in which the physician can program the robot’s computer to select grafts from areas of higher density and avoid those of lower density in advance of the actual extraction. It can also increase the spacing of the harvests in areas of lower density and can feather the edges of the harvest for a more undetectable appearance. Although these manipulations can be done by hand, with the robotic system the physician can make these decisions in advance. In this way, the process is not affected by decreased visibility due to bleeding or the loss of orientation and/or concentration when the manual operator is focused on other factors such as punch angle and depth.
In manual FUE techniques, hand-held instrumentation can vary from sharp punches to dull instruments and these can be motorized to rotate into the skin or manually oscillated. The physician wears magnifying lenses to directly visualize the hair on the scalp, manually aligns the cutting tip of the extraction instrument to be parallel to the hair follicles as it penetrates the skin and physically estimates the depth of the punch, or controls it with a mechanical stop. In the manual system, graft selection is achieved visually by the physician.
Recipient Site Creation
When recipient site creation is performed manually, the physician must estimate both the distribution and density of sites for a specific area. He must then control both the angle and depth as these sites are being made, as well as trying to avoid existing terminal hair.
In robotic site creation, the physician first uses a software program on a tablet computer to design the recipient site pattern on a 3D model of the actual patient. Once the physician and patient agree on a plan, the treatment plan is transferred to the robotic system. The physician programs the system so that a specific number of grafts can be randomly distributed over the desired area, eliminating errors in placing too many grafts in one area and having inadequate numbers for another. The robotic system can also be more uniform in site depth and more precise in keeping sites parallel to one another compared to hand. Most importantly, when creating sites in areas of existing hair, the robot can be programmed to avoid pre-existing terminal hair by a pre-determined distance – a task that is extremely difficult to do by hand.
In sum, the robotic FUE system can perform both the separation of follicular unit grafts from the surrounding scalp and recipient site creation with precision and consistency, regardless of the number of grafts. Its image-guided system and sophisticated computer algorithms enable the physician to carry out these functions to his/her exact specifications, but can also be adjusted in real-time as the clinical situation demands.
Read more about the advantages of Robotic FUE over traditional manual FUE procedures.
There are four main steps to a Follicular Unit Extraction (FUE) procedure (in addition to the consultation, surgical planning and design). These are:
- Separation of follicular unit grafts from the surrounding scalp
- Extraction of the grafts from the scalp, trimming and sorting
- Recipient site creation
- Graft placement
The ARTAS robot, under the guidance of a hair transplant surgeon, can perform two of the four major steps in an FUE hair transplant: follicular unit separation (step 1) and recipient site creation (step 3).
After follicular unit grafts have been separated from the surrounding tissue by the robot, they are manually extracted using fine, serrated forceps. The extracted grafts are then trimmed, counted, and sorted according to the number of hairs they contain (step 2). The robot is currently not able to perform these steps.
It is anticipated that within the next several years, the robotic system will be able to make recipient sites and simultaneously place grafts into these sites (steps 3 & 4), so that in the near future, three of the four main steps of FUE will be performed robotically.
In a Follicular Unit Extraction (FUE) procedure, the physician should be intimately involved with the entire hair transplant, whether manual or robotic. In robotic graft extraction, the physician inputs the surgical parameters into the robot’s software via a computer terminal or hand-held device. At the start of the procedure, he manually applies the tensioner (a rectangular picture frame-like device) to the patient’s scalp to orient the robot in the operative field and to create traction on the scalp. During the procedure, the physician can adjust certain parameters, such as punch depth and angle, using the hand-held pendant or the computer. The tensioner must also be advanced to new areas of the scalp as the harvest in each area has been completed.
In robotic site creation, the physician programs the total number of sites, density for specific areas, site angle, needle orientation (coronal or sagittal) and site depth. A fiducial is used to orient the robot to specific regions of the patient’s scalp. Once programmed, the site creation will proceed automatically unless overridden by the physician.
There are many other important physician-dependent steps in the Robotic FUE hair transplant, especially the recipient site planning and design of the procedure. Other steps, such as the microscopic sorting and trimming of harvested follicular unit grafts and graft placement, are often performed by trained staff, but require the physician’s close supervision.
As with manual FUE, robotic FUE hair transplantation is a minimally-invasive outpatient procedure performed under long-acting local anesthesia – usually a combination of lidocaine and bupivacaine. After the initial injections, the patient doesn’t experience any pain or discomfort. In contrast to an FUT-strip procedure which can be uncomfortable in the donor area for days to weeks following surgery, with robotic FUE, there is no discomfort once the procedure is completed and the anesthesia wears off.
All Follicular Unit Extraction procedures produce donor scarring, but in contrast to the linear scar of an FUT-strip, FUE procedures leave fine, white dots easily covered by hair. Scarring from robotic FUE is comparable to scarring from manual FUE for similar size punches. Scarring can be minimized with robotic FUE by programming the robot to select only the larger follicular units so that there will be more hair, on average, obtained per harvest.
ARTAS Hair Studio is a computer program that allows physicians to help patients see his/her personalized hair restoration outcome through a visualization of the planned results. The software creates a 3-D digitized model of the person’s head which can be used to demonstrate how the results will appear. The physician can even show the patient anticipated results using different numbers or densities of grafts. The software also aids the physician in explaining important details of the transplant design. As a result, the patient is more engaged in the process and can better understand the rationale behind the surgeon’s recommended plan.
If the physician controls the robotic procedure, there should be no more risk than if the physician performed the entire procedure manually. The ARTAS system is a 510K cleared medical device that was engineered to include multiple safety features including automatic optical control, force sensors, and E-stops. The tensioner, a frame-like device that is applied to the patient’s scalp, is secured with silicone straps that limit head motion during the procedure. If there is any head movement while the robot is functioning, built in motion sensors automatically pause the action of the robotic arm. The robot can also be paused at any time using the stop buttons located on the pendant and at the computer user interface.
Another safety feature of the robot is the system of sensors that determine the depth of punches used in harvesting and the needles in recipient site creation. If a sensor registers forces beyond safety threshold levels or increasing forces during dissection, an automatic stop is triggered and the device retracted away from the scalp.
We do not use ARTAS technicians at Bernstein Medical. The staff members that assist Dr. Bernstein or Dr. Wolfeld during the robotic FUE procedure are our regular full-time staff of nurses and medical assistants who are fully trained and certified in the ARTAS procedure. Because we also perform FUT, our staff is also expert in stereo-microscopic follicular unit dissection, an essential part of trimming, counting and sorting the robotically-harvested grafts.
The Neograft machine for Follicular Unit Extraction (FUE) uses a single sharp punch to isolate grafts and a suction mechanism to extract grafts from the scalp. Both the sharp punch and suction are felt by many doctors to risk injury to the follicles due to the tendency to cut follicles and separate the follicles from their vital support tissue. Also, the Neograft uses a hand-held instrument that must be manually guided by the physician in order to extract the grafts. If the physician imperfectly aligns the sharp punch with a follicular unit or if the incision is too shallow, there is a significant risk of damaging the graft. The ARTAS robot‘s two-step sharp/blunt dissection technique and image-guided robotic system offer precision and control that is impossible to replicate using a hand-held FUE device like the Neograft.
The ARTAS FUE robot has multiple safety features that are only available in a robotic system. The tensioner, or grid, that is applied to the patient’s scalp is secured with silicone straps that limit head motion during the procedure. If there is any head movement while the robot is functioning, built in motion sensors automatically pause the action of the robotic arm. The robot can also be paused at any time using the stop buttons located on the pendant and at the user interface.
Another important safety feature of the robot is the system of advanced sensors that determine the precise depth of the sharp and blunt needles used in the punching mechanism. These needles each have a built-in skin pressure sensor that can trigger an automatic on/off switch. If a sensor registers pressure greater than 10 newtons, an automatic stop is triggered and the punch mechanism is retracted.