Q: Can you use a hair transplant to treat radiation-induced permanent hair loss in pediatric patients?
A: Yes, but there are a number of things to consider:
- As in adults, if the hair loss from radiation is extensive, or involves the permanent zone of the scalp, there would not be enough donor hair to make the procedure worthwhile.
- Depending on the nature of the scarring, it may not take grafts well and always will require multiple procedures to achieve adequate density.
- Hair transplant procedures (both FUT and FUE) leave scarring, so future treatments for tumor recurrences that cause hair loss (radiation or chemo) may expose these scars and be an additional cosmetic problem.
- There is a concern that the younger patient may eventually develop androgenetic alopecia and this would be a problem if extensive and occurring early. Family history, of course, is important, but there is no way to tell with certainty the prognosis of AGA in a young person.
- For those that might develop AGA, finasteride is not indicated in males under 18 and there is no way to tell in advance if the person can tolerate this medication.
- The hair transplant procedure is long, so local rather than general anesthesia is used. That said, 12 y/o is generally the minimum age that a patient can tolerate the procedure and a 12 y/o needs to be mature and motivated. Certainly, waiting until the patient is older makes it easier surgically.
Q: What is Lichen planopilaris? — G.S., Pleasantville, NY
A: Lichen planopilaris (LPP) is a distinct variant of cicatricial (scarring) alopecia, a group of uncommon disorders which destroy the hair follicles and replace them with scar tissue. LPP is considered to have an autoimmune cause. In this condition, the body’s immune system attacks the hair follicles causing scarring and permanent hair loss. Clinically, LPP is characterized by the increased spacing of full thickness terminal hairs (due to follicular destruction) with associated redness around the follicles, scaling and areas of scarred scalp. In contrast, in androgenetic alopecia (AGA) or common baldness, one sees smaller, finer hairs (miniaturization) and non-inflamed, non-scarred scalp. Complicating the picture is that LPP and AGA can occur at the same time – particularly since the latter condition (common baldness) is so prevalent in the population (see photo). And LPP can involve the frontal area of the scalp, mimicking the pattern of common genetic hair loss. Interestingly, the condition is more common in women than in men.
For those considering a hair transplant, ruling out a diagnosis of LPP is particularly important as transplanted hair will often be rejected in patients with LPP. In common baldness, the disease resides in the follicles (i.e., a genetic sensitivity of the follicles to DHT). Since the donor hair follicles remain healthy, even when transplanted to a new location, we call common baldness donor dominant. It is the reason why hair transplantation works in persons with common baldness. In contrast, LPP is a recipient dominant condition. This means that the problem is in the recipient area skin, so if healthy hair is transplanted into an area affected by LPP the hair may be lost.
Because it is so important to rule out suspected LPP when considering a hair transplant and because it is often hard to make a definitive diagnosis on the physical exam alone, a scalp biopsy is often recommended when the diagnosis of LPP is being considered by your doctor. A scalp biopsy is a simple five minute office procedure, performed under local anesthesia. Generally one suture is used for the biopsy site and it heals with a barely detectable mark. It takes about a week to get the results. The biopsy can usually give the doctor a definitive answer on the presence or absence of LPP and guide further therapy. If the biopsy is negative, a hair transplant may be considered. If the biopsy shows lichen planopilaris, then medical therapy would be indicated.
Q: I am suffering from Pseudopelade for four years now. I have lost a lot of hair & there are big bald patches on the top of my scalp that are difficult to hide. Is there any hair transplant surgery or follicle transplant surgery possible in my case, or anything else I can do? — T.L., Boston, MA
A: In general, hair transplantation does not work for Pseudopelade (a localized area of scarring hair loss on the top of the scalp) since the condition is recipient dominant rather than donor dominant.
With a donor dominant condition, such as androgenetic hair loss, the tendency to have the condition, or be resistant to it, is located in the hair follicle and moves with the hair follicle when the follicle is transplanted to a new area. Therefore, in androgenetic alopecia, healthy permanent hair taken from the donor area in the back of the scalp will continue to grow in the a new location in the balding part of the scalp.
In a recipient dominant condition, such as Pseudopelade, the problem is in the skin, so if you perform a hair transplant into an affected area of skin, the transplanted hair will become affected by the same process and be lost.
The disease process can often be slowed down with anti-inflammatory agents, such as corticosteriods, applied or injected locally and the bald area can be camouflaged with cosmetics specially made for use on the scalp. See the Cosmetic Camouflage Products page on the Bernstein Medical – Center for Hair Restoration website.
Q: I am a 34 year woman with a patch of hair loss by my temple. I went to the salon to have my hair done and to my surprise my hairdresser told me that I have Alopecia? First time I’d heard of it, my G.P is not very concerned about it but having read so much about it on this site I am becoming a bit concerned. The rest of my hair is healthy any suggestions and diagnosis? — M.V., Williamsburg, Brooklyn
A: “Alopecia” is just a generic term for any kind of hair loss.
It sounds like you have a specific condition called alopecia areata. Alopecia areata is an autoimmune disease that presents with the sudden appearance of well localized bald spot(s) on the scalp or other parts of the body. The underlying skin is always normal.
The treatment is injections with cortisone. Hair transplant surgery is not indicated for this condition.
You should see a dermatologist to confirm the diagnosis and treat.
Other diagnoses to consider are triangular alopecia (which would have been present since childhood) and traction alopecia (that is cased by constant tugging on the hair).
Q: One of the things that I have noticed as a person who has needed to take thyroid medication for a long, long time, is that when my thyroid gets a little bit out of balance – when I’m not getting quite enough, I begin to notice is that my hair starts falling out. What about the role of thyroid for hair loss? — T.K., Mineola, NY
A: Both increases and decreases in thyroid levels can cause hair loss and changes in the levels of thyroid hormone can change the consistency of one’s hair. Elevated hormone levels cause scalp hair to be fine and soft, with diffuse thinning being relatively characteristic.
When thyroid hormone levels are low, the hair becomes dry, coarse, and brittle. Hair loss can be either patchy or diffuse (involving the entire scalp).
Low levels of thyroid hormone are associated with the loss of the outer 1/3 of the eyebrows and a decrease in body hair. When changes in thyroid hormone levels are abrupt, there can be dramatic shedding (telogen effluvium).
The most important thing to do if you have thyroid disease is to try to keep the levels within a normal range and keep them as steady as possible. If you are taking thyroid medications, try to use them on a regular basis, because alterations of ones in hair can be caused by large fluctuations in the levels, as much as by the absolute values.
Q: Can a hair transplant into bald areas caused by alopecia areata ever be successful? — R.K., Providence, R.I.
A: Alopecia areata is an autoimmune disease in which the body attacks its own hair follicles. It generally appears as round patches of smooth bald areas scattered in the scalp or beard. Less commonly, it can involve the entire scalp (alopecia totalis) or all facial and body hair (alopecia universalis). Unless the condition is well localized and totally stable, hair transplantation is not likely to be effective because the transplanted hair would be subject to the same problem.
We prefer that one have no new lesions for a minimum of two years before considering surgical hair restoration, although this does not ensure that the procedure will be successful.
You may find more information on this relatively common condition at the National Alopecia Areata Foundation (NAAF). For more information, visit: www.naaf.org.
Browse Hair Restoration Answers by topic:
Learn more about hair restoration
Hair loss has a variety of causes. Diagnosis and treatment is best determined by a board-certified dermatologist. We offer both in-person and online photo consults.
Provide your email to learn more.


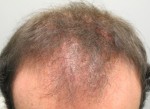 LPP in Male Pattern Alopecia
LPP in Male Pattern Alopecia


