Dr. Bernstein was interviewed by Skin & Allergy News in their article, “Microscopic Dissection Offers Superior Yield” The complete article is below:
Skin & Allergy News
February 1999

Microscopic Dissection Offers Superior Yield
Articles by Anna Nidecker
Senior Writer
Washington — The dissecting microscope takes some getting used to, but using it makes more efficient use of donor hair during follicular unit transplantation than magnifying loupes with transillumination, reported Dr. Robert Bernstein of Columbia University 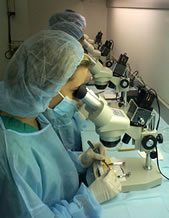 College of Physicians and Surgeons, New York.
College of Physicians and Surgeons, New York.
“A limiting factor in all hair restoration surgery is the patient’s finite donor supply. […] Meticulous stereomicroscopic dissection should help preserve the supply and ultimately provide the patient with the most transplantable hair,” he said at the annual meeting of the International Society of Hair Restoration Surgery.
Dr. Bernstein compared the follicular unit graft yields of dissections performed with stereoscopic microscopes and with loupes and backlighting. Initial sectioning of the intact strip was done with loupes, as the staff had not yet mastered the skill of slivering that is needed to section the intact strip under microscopic guidance.
“This method may be useful for a team in transition, a model for staffs in transition to using the microscope,” the hair transplant surgeon suggested.
Tips on Transition to Microscopes
The microscope offers a better yield with follicular transplantation, but some doctors feel that abruptly switching from loupe magnification may send an office into turmoil.
Microscopes will be well received by staff if they clearly understand the benefits and are eased into the transition, Dr. Bernstein said.
Dr. David Seager advised physicians planning the transition to the use of microscopes to let staff observe microscopic dissection at another clinic with an established program, and to send them somewhere to be trained before they start. The Toronto hair transplant surgeon also advised buying a couple of microscopes and letting the staff “play” with them for a while, cutting at their own leisurely rate before entering into a high-pressure transplant session.
Dr. Bernstein also recommended easing slowly into the transition by first training a small portion of staff, which will not affect the overall time of surgery.
Another option is to hire a couple of new technicians and train them from the beginning with microscopic dissection, Dr. Seager suggested.
“You’ll be amazed at the beautiful grafts they will be cutting in a couple of weeks. […] It may be only 40 grafts an hour, but these newcomers will be cutting better grafts than even your 8-year veterans,” he said. “Old staff will look at these new technicians and their grafts, and, if they take pride in their work, they will be quite jealous and will be really eager to catch up.”
Dr. Bernstein agreed: “The value of the microscope may be more significant in the hands of less experienced dissectors. […] There’s some advantage even at the outset.”
Continued resistance from staff should be met with a deadline: ‘Anyone who can’t or won’t fit in, tell them they can do something else in the office, but they won’t be doing transplanting,” Dr. Seager said.
In 41 patients, the donor strip was harvested with a double-bladed knife from the midportion of the permanent zone in the back of the scalp.
The strip was divided into two equal parts along the midline; these were further divided into 2- to 3-mm wide vertical sections using loupes and a straight razor. Sections from one of these donor strip halves were further dissected into follicular units using a 10x power microscope; sections from the other donor strip half were dissected using magnifying loupes.
Follicular units cut using the microscope contained an average of 2.41 hairs; those cut using loupe magnification yielded 2.28 hairs. Use of the microscope also yielded 10% more follicular units and 17% more hair overall, compared with use of loupes.
The grafts were dissected and sorted into follicular units containing one to four hairs, and all hair and hair fragments judged to be potentially viable were counted towards the yield (Dermatol. Surg. 24[8]:875-80, 1998).
Microscopic dissection took from two to four times as long as loupe magnified dissection when technicians first began using the microscopes. After 3 months, the procedure still took twice as long with the microscopes. But by the end of the study 1 year later, it took only 10% longer, a rate they currently maintain, Dr. Bernstein said.
Hand-eye coordination was a factor which automatically improved, and the inefficient movement of grafts in and out of the microscopic field was solved with better organization, he said. Technicians with a tendency to obsessively sculpt grafts under the microscope can be educated to limit this sculpting, which does not affect the quality of the transplant.
Use of the microscope also led to fewer reports of back and neck strain by assistants. They also reported easier dissection when there was donor scarring, and with blond or light-colored hair.
Besides the benefit at the stage of dissecting the sections—as shown in this study—microscopes can improve yield by 5%-10% at the “slivering” stage. Yield can be improved an additional 15%-20% by avoiding use of the multibladed knife at the donor harvesting stage.
Loupe advocates argue that microscopes unduly slow down the procedure and that staff resistance to this new technology may be an insurmountable problem in some practices. They also lament the higher economic cost of purchasing the microscopes, training the staff, and slowing down dissection time with no clear benefits.
Dr. Bernstein said that the benefits of microscopic dissection far outweigh these minor inconveniences and should be incorporated into hair transplant procedures.
Posted by Robert M. Bernstein M.D. 


 The Trustees of Columbia University have named Dr. Bernstein, hair transplant pioneer, the Clinical Professor of Dermatology. This promotion was based on Dr. Bernstein’s teaching, lectures, research, original scientific papers, and outstanding patient care.
The Trustees of Columbia University have named Dr. Bernstein, hair transplant pioneer, the Clinical Professor of Dermatology. This promotion was based on Dr. Bernstein’s teaching, lectures, research, original scientific papers, and outstanding patient care. The
The 
 College of Physicians and Surgeons, New York.
College of Physicians and Surgeons, New York. Robert M. Bernstein, MD, is Medical Director of the New Hair Institute Medical Group in New York. He is Assistant Clinical Professor of Dermatology at the college of Physician and Surgeons of Columbia University, and an Associate in the Dermatology Service at the Columbia Presbyterian Medical Center, where he teaches dermatologic and laser surgery, and hair transplantation. He is also an attending physician in dermatology at Englewood Hospital and at the Manhattan Eye, Ear and Throat Hospital.
Robert M. Bernstein, MD, is Medical Director of the New Hair Institute Medical Group in New York. He is Assistant Clinical Professor of Dermatology at the college of Physician and Surgeons of Columbia University, and an Associate in the Dermatology Service at the Columbia Presbyterian Medical Center, where he teaches dermatologic and laser surgery, and hair transplantation. He is also an attending physician in dermatology at Englewood Hospital and at the Manhattan Eye, Ear and Throat Hospital.



