Pages:
&after=
&link_before=&link_after=‘); ?>
PROBLEMS AND COMPLICATIONS
The use of large numbers of very small grafts, particularly follicular units, that became popular in the latter half of the 1990’s, eliminated many of the problems encountered with the older plug procedures. With “modern” hair restoration techniques, however, problems still remain. These problems can be grouped into one of four broad categories; those caused by: 1) poor patient selection, 2) poor aesthetic judgment, 3) improper handling of grafts, and 4) wide donor scars. These issues have been discussed in the body of this paper so just a few points will be emphasized.
Poor Patient Selection
Probably the most common error in hair transplantation is poor patient selection, particularly operating on patients who are too young. Since the goal of a young person is to restore his adolescent hairline, transplanting a patient who is too young, almost invariably leads to creating a hairline that is too low and/or too broad. And since a low, broad hairline is also associated with normal density, as the person ages (and his total hair volume decreases) re-distributing hair through hair transplant surgery will not be able to make the person’s hair look natural long-term. An attempt to provide coverage to a Norwood Class 6 or 7 patient, who has a permanent low, broad hairline, will result in a diffusely thin, non-patterned, look.
If a person younger than 23-25 is transplanted, it is important to place the hairline in a mature position (i.e. at least 1.5cm above the upper brow crease), create significant temple recession, and be reasonable certain that the patient does not have diffuse unpatterned alopecia (DUPA), i.e. that he has a stable permanent zone with no significant miniaturization. Since this design will rarely satisfy the younger patient, and since the stability of the donor area can rarely be know for certain at this age, the other alternative, waiting until the patient is more mature before undergoing hair restoration surgery, is usually the more appropriate route.
It had been felt by some that the new, more effective hair loss medications, such as finasteride, will allow the surgeon to be more aggressive in operating on a younger patient. It is the opinion of these authors that the real value of these medications in the younger patient lies in their ability to postpone, rather than expedite, the decision to have hair transplant surgery.
Poor Aesthetic Judgment
One of the most common aesthetic mistakes is to place grafts radially along the frontal hairline, rather than in a forward direction. Unfortunately, grafts placed in the wrong direction (as well as those placed too low in the hairline) must be removed, since camouflage with additional hair will not correct the problem. The most satisfactory treatment in these cases is often laser hair removal since, with the advent of micrografting and follicular unit transplantation, the grafts are often too small and too numerous to be individually excised and re-used. This results in wasted time and expense for the patient and, of course, the unnecessary loss of donor hair. The issue will be discussed in the section Corrective Procedures.
Another common error is to transplant the crown in a young person, or in a person who is just starting to thin in the vertex and who may become extensively bald. The procedure often accelerates hair loss in this area and commits the hair restoration surgeon to performing multiple, small procedures to follow the expanding crown. This can leave the patient’s donor reserves in short supply to address the frontal hairline, front and top part of the scalp, as the balding extends to these cosmetically more important areas.
Poor Growth
The nuances of graft handling are beyond the scope of this writing, nevertheless, improper handling of grafts is a major cause of poor grow and the reason that particular aesthetic goals are often not met. There are certain key points to consider if one is to have maximum graft survival. These are:
- Grafts are subject to injury from the moment they leave the donor area until they are totally secure in the recipient scalp (up to 8 days post-op).
- The staff must be continually supervised to insure that optimal graft handling is maintained through the entire procedure.
- Damage to grafts can be caused by mechanical injury (transection during dissection or crush injury from improper use of forceps during placing), dehydration, chemical solutions (such as concentrated hydrogen peroxide), heat (from the OR lights or dissecting microscope) and hypoxia (from keeping the grafts out of the body too long.11,12
- Of the various forms of injury, desiccation is the most damaging and can place the grafts at greater risk of other forms of injury.11
Wide Donor Scars
With the use of smaller grafts, having a pluggy look is no longer a major concern for hair transplant patients and the fear of having a widened donor scar has come to the forefront. Although legitimate, this concern has been exacerbated by the frequent scarring that occurred from the older techniques, by inexperienced doctors harvesting donor strips that are too large (in an attempt to perform megasessions), by the those hoping to exploit the fear of linear donor scars to promote non-surgical methods or follicular unit extraction, and by a complication being occasionally broadcast over the internet.
As with progress in the recipient area, achieved through the use of follicular units, there has been significant progress in our understanding of how to keep donor scars thin. These include:
- Noting a history of stretched scars from other procedures
- Carefully assessing scalp laxity to judge the width of the donor incision
- Limiting the width donor incision to 1.0-1.2 cm. for most patients to insure a low tension closure
- When appropriate, decreasing the donor width in subsequent procedures
- Harvesting from the mid-portion of the permanent zone for the following reasons:
- the muscle movements of the neck will be transferred to low incisions and increase the risk of stretch
- the hair around high donor incisions many not be permanent and may expose the scar
- the hair removed in a high donor incision transplanted into the donor area may be lost over time
- Using tumescent anesthesia to keep the donor incision superficial, i.e. in mid fat, so that it is below the follicles but above the fascia and major neurovascular bundles.
- Waiting at least 6-8 months between procedures to allow for the wound to be completely healed and some donor laxity to return.
Complications encountered in hair transplantation are infrequent. They include some of the problems seen with other minor out-patient surgical procedures such as: syncope from vaso-vagal reactions; anxiety, palpitations and hypertension from the epinephrine in the local anesthetic; hypotension from epinephrine-beta blocker interactions; post-op bleeding from improper suturing or coagulopathies; bacterial infections from intra-operative or post-op contamination; and a thickened donor scar from poor suturing techniques or factors intrinsic to a particular patient. If the local anesthetic is administered improperly, or in too high a dose, lidocaine toxicity can result. Rarely a patient may have an allergic reaction to the anesthetic or other medications administered during the hair restoration surgery.
There are a number of problems that are more specific to hair transplantation. Post-op facial edema, that begins at the hairline and then settles into the bridge of the nose, is so common that is should be consider an intrinsic part of the procedure. Fortunately, it generally mild and resolves within a week. There is some evidence that systemic corticosteroids can decrease the severity of the swelling.
Persistent numbness or paresthesias in the occipital scalp, which were once a common problem in hair transplant surgery, have been virtually eliminated by the use of tumescent anesthesia, as this helps to confine the depth of the donor incision to the subcutaneous space. Interestingly, the incidence of post-op hiccups, a complication attributed to injury of cervical nerves C2-C4, indirectly simulating the vagus or diaphragmatic nerves, has also markedly diminished with the use of tumescence and more superficial donor incisions.
A sterile folliculitis not uncommonly occurs from 1-4 months post-procedure, as the new hair attempts to negotiate its way to the scalp surface, but gets trapped in the epidermal overgrowth at the follicular orifice. These lesions usually subside spontaneously without treatment. Occasionally they will become secondarily infected and require antibiotics or form a cyst that needs to be incised and drained.
Hair texture changes most likely result from the trauma associated with graft dissection and placement. It is less common with meticulously performed follicular unit transplantation and, in contrast to the permanent texture changes seen in large graft transplants, it is almost always transient. Skin texture changes are almost never seen in follicular unit hair transplantation if the recipient wound are kept to the equivalent of a 19- or 20-guage needle at the hairline and an 18-gauge site overall.
Hair loss in the donor area can occasionally result from an excessively tight wound closure, particularly when the tension is increased by significant post-op edema. Hair loss in the immediate vicinity of the incision is more common. This can by be caused by the entrapment of hair follicles within wide suture bites or by an inflammatory reaction to the suture material.
Some degree of hair loss in the recipient area, in the vicinity of the transplant, is so common that it, like post-op edema, should be considered an intrinsic part of the hair restoration procedure. The mechanism is felt to be telogen effluvium, however, when miniaturized hair is shed, it often will not return, giving the appearance of a progression of the hair loss. Finasteride may offer some protection against this process, but this has not been proven. The physician should anticipate hair loss by avoiding performing a transplant too early. When the procedure in undertaken the surgeon should transplant enough hair to compensate for any potential loss. The important point is that the patient should be made aware of this aspect of a hair transplant and be told that, even in a perfectly executed procedure, at least some small degree of hair loss is the rule, rather than the exception.
CORRECTIVE PROCEDURES
Traditionally, hair transplant surgeons have attempted to improve the appearance of larger grafts by placing a zone of smaller grafts in front of them. This had been an integral part of the doctor’s strategy, when he/she used large grafts in the central scalp for density and smaller grafts around the perimeter for naturalness. Often, however, the end result was still unnatural. As an extension of the original thinking, additional sessions of small grafts were added to the initial ones in the hope of further improving the appearance of the larger grafts. (Figure 19)
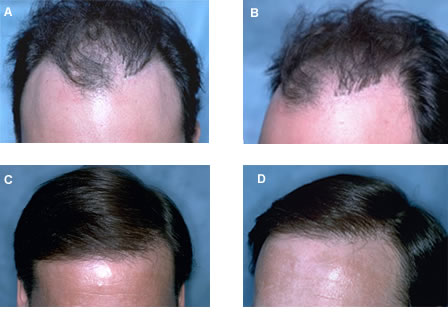 Figure 19. (A,B). Before views of a patient treated with rows of grafts placed in his temples. These grafts became visible as his hairline receded. (C,D) The patient was treated with just one session of follicular unit transplantation as the larger grafts were far enough behind the transplanted hairline to be camouflaged.
Figure 19. (A,B). Before views of a patient treated with rows of grafts placed in his temples. These grafts became visible as his hairline receded. (C,D) The patient was treated with just one session of follicular unit transplantation as the larger grafts were far enough behind the transplanted hairline to be camouflaged.A major shift in the approach to these hair restoration patients came from the realization that camouflage alone is rarely adequate for restoring a natural appearance, particularly if the original grafts were too large, too far forward on the hairline, or pointing in the wrong direction. In these situations, only partial or complete excision of the original grafts would correct the problem. In fact, when the grafts are in the wrong position or direction, rather than just too large, their complete removal is generally the best option.39,40
Grafts can be removed by either excising them, through punch or linear excision, or by removing the hair alone, via laser hair removal or electrolysis. When making a decision regarding the best way to remove the grafts, one should consider the quality of the underlying skin, as well as the actual hair in the grafts. If the underlying skin is appears normal, then removing the hair alone may be the best choice.
One must also decide before hand where to place the hair that will be obtained from the grafts. If that patient wants to completely reverse the transplant, rather than repair existing grafts, and move forward with additional transplants after the correction, one should consider placing the hair back into the donor area.
If the patient wishes to proceed with further hair transplant procedures, the hair that is obtained from the plugs should be placed in an area that requires additional density (such as the central forelock area), but this hair should not be place at the frontal hairline, since the hair obtained from plugs can be more wiry than hair taken form virgin scalp. If the patient has little, or no, donor reserves, then even the hair derived from the grafts should be used in the cosmetically most important areas, i.e. the hairline.
When the grafts have been placed close together, are in multiple rows, or are very large, multiple graft excision sessions are often needed. The surgeon should wait a minimum of eight weeks between these sessions to give time for the area to heal and to allow for the identification of any missed or transected follicles that might regrow. When possible, it best to complete all the repair sessions requiring graft excision before additional donor hair is used, so that the graft excisions will not be encumbered by the additional hair. By waiting for the repairs to be complete, the doctor can easily visualize where to place the remaining donor hair and may have the option of using some of the additional hair to cover surface irregularities that have been uncovered by the graft excisions. (Figure 20)
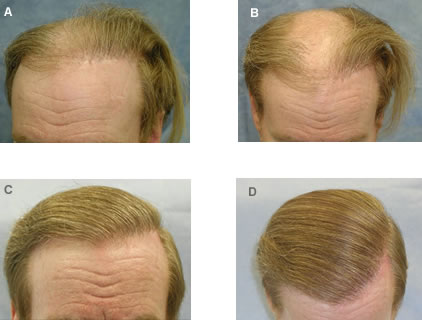 Figure 20. (A,B) Before views of a patient with a rim of plugs, central baldness and a markedly depleted donor supply. (C,D) Four corrective procedures were performed to remove the large grafts and redistribute them as individual follicular units in the front part of his scalp. In the fifth procedure, 1,184 follicular units were transplanted from the donor area into the front and mid-portion of his scalp. Although he still relies on a comb-over to add fullness to the top part of his scalp, note the natural appearance of the hair restoration.
Figure 20. (A,B) Before views of a patient with a rim of plugs, central baldness and a markedly depleted donor supply. (C,D) Four corrective procedures were performed to remove the large grafts and redistribute them as individual follicular units in the front part of his scalp. In the fifth procedure, 1,184 follicular units were transplanted from the donor area into the front and mid-portion of his scalp. Although he still relies on a comb-over to add fullness to the top part of his scalp, note the natural appearance of the hair restoration.A detailed discussion of repair work may be found in references 39 and 40. The following are key points to consider when performing corrective procedures:
- Although it is more time consuming, patients will get a better cosmetic result if the grafts are sutured closed than if they are left to heal by secondary intention.
- Grafts that are too large can be partially removed as long as they are in the central scalp and pointing in the proper direction.
- Grafts that are in the wrong position, or pointing in the wrong direction, should be completely removed.
- Punch excision, although more time consuming, usually gives a better cosmetic result than a linear excision.
- For micrografts and follicular units that are pointing in the wrong direction, or that have been placed too far forward, laser hair removal is generally the best option.
- It is best to complete the removal phase of the repair before additional hair is taken from the donor area.
SUMMARY
The recognition that the follicular unit is a discrete, anatomic and physiologic entity, and that preserving it through stereo-microscopic dissection is the best way to ensure the naturalness of the restoration, has brought hair transplant surgery into the twenty-first century. Issues yet to be resolved include: determining the maximum density and number of grafts that can be safely used in a single session, finding the ideal rotational orientation of the grafts, deciding whether it is preferable to pre-make recipient sites or immediately place grafts into sites as they are made, and defining the precise role of follicular unit extraction.
Regardless of how these issues are ultimately resolved, the essence of providing the best care for patients will continue to rest on proper patient selection, establishing realistic expectations, and using non-surgical management for young persons who are just starting to thin. When hair transplantation is indicated, it should be accomplished in larger, rather than small sessions and be performed by a team experienced in the dissection and handling of the thousands of tiny follicular unit grafts needed to accomplish the hair restoration. Only with meticulous attention to every aesthetic and technical detail can the best cosmetic result be assured.
References
1. Limmer BL. Elliptical donor stereoscopically assisted micrografting as an approach to further refinement in hair transplantation. Dermatol Surg 1994; 20:789-793.
2. Bernstein RM, Rassman WR, Szaniawski W, Halperin A. Follicular transplantation. Intl J Aesthetic Rest Surg 1995; 3:119-132.
3. Bernstein RM, Rassman WR: Follicular transplantation: patient evaluation and surgical planning. Dermatol Surg 1997; 23:771-784.
4. Bernstein RM, Rassman WR: The aesthetics of follicular transplantation. Dermatol Surg 1997; 23:785-799.
5. Headington JT. Transverse microscopic anatomy of the human scalp. Arch Dermatol 1984; 120:449-456.
6. Bernstein RM, Rassman WR: The logic of follicular unit transplantation. Dermatologic Clinics 1999; 17(2):277-295.
7. Windam C. Beyond the Comb-Over. The Wall Street Journal, New York, NY, November 11, 2003. pg D1.
8. Unger WP, Shapiro R. Hair transplantation. New York: Marcel Dekker; 2004.
9. Seager D: Binocular stereoscopic dissecting microscopes: should we use them? Hair Transplant Forum International 6:(4):2-5, 1996.
10. Beehner ML. A study comparing growth of “intact” FUs and “non-intact” grafts. Hair Transplant Forum International 13:(6):461-2, 2003.
11. Gandelman M, et al: Light and electron microscopic analysis of controlled injury to follicular unit grafts. Dermatol Surgery 2000; 26(1): 31.
12. Greco J: The H-factor in micrografting procedures. Hair Transplant Forum International 6 :(4):8-9, 1996.
13. Limmer B: Thoughts on the extensive micrografting technique in hair transplantation. Hair Transplant Forum International 6:(5):16-18, 1996.
14. Rassman WR, Bernstein RM, McClellan R, Jones R, et al. Follicular Unit Extraction: Minimally invasive surgery for hair transplantation. Dermatol Surg 2002; 28(8): 720-7.
15. Bernstein RM, Rassman WR, Anderson KW: Follicular Unit Extraction Megasessions: Evolution of a technique. Hair Transplant Forum International 2004; 14(3): 97-99.
16. Kuster W, Happle R. The inheritance of common baldness: two B or not two B? J Am Acad Dermatol 1984;11:921-926.
17. Norwood OT. Male pattern baldness: classification and incidence. So Med J 1975; 68:1359-1365.
18. Bernstein RM, Follicular Unit Hair Transplantation. In: Robinson JK, Hanke CW, Siegel DM, Sengelmann RD, editors: Surgery of the Skin, Chapter 34. Elsevier Mosby Inc., London UK. 2005.
19. Bernstein RM, Rassman WR: The scalp laxity paradox. Hair Transplant Forum Intl 2002; 12(1):9-10.
20. Beehner M. Nomenclature proposal for the zones and landmarks of the balding scalp. Dermatol Surg 2001; 27:375-380.
21. Bernstein RM, Rassman WR, Seager D, Shapiro R, et al. Standardizing the classification and description of follicular unit transplantation and mini-micrografting techniques. Dermatol Surg 1998; 24:957-963.
22. Smith JB, Fenske NA. Cutaneous manifestations and consequences of smoking. J Am Acad Dermatol 1996; 34:717-32.
23. Haas A, Grekin R. Antibiotic prophylaxis in dermatologic surgery. J Am Acad Dermatol 1995; 32:155-176.
24. Bernstein RM, Rassman WR. Dissecting microscope versus magnifying loupes with transillumination in the preparation of follicular unit grafts: a bilateral controlled study. Dermatol Surg 1998; 24:875-880.
25. Limmer BL. Micrograft survival. In: Stough DB, Haber, RS, eds. Hair replacement: surgical and medical. St. Louis: Mosby; 1996:147-149.
26. McCaughey W. Adverse effects of local anesthetics. Drug Safety 1992; 7:178-189.
27. Bernstein RM, Rassman WR: Hemostasis with minimal epinephrine. Hair Transplant Forum Intl 1999; 9(5):153.
28. Skidmore R, Patterson J, Tomsick R. Local anesthetics. Dermatol Surg 1996; 22:511-522.
29. Weiner N, Norepinephrine, epinephrine, and the sympathomimetic amines. In: Goodman AG, Gillman LS. The pharmacological basis of therapeutics, 7th ed. Chapter 8:151-159. New York: Macmillan; 1985.
30. Bennett RG: Selection of wound closure materials. J Am Acad Dermatol 1988; 18:619-637.
31. Moy RL, Waldman B, Hein DW: A review of sutures and suturing techniques. J Dermatol Surg Oncol 1992; 18:785-795.
32. Bernstein RM, Rassman WR, Rashid N: A new suture for hair transplantation: Poliglecaprone 25. Dermatol Surg 2001; 27(1):5-11.
33. Seager, D. The ‘one-pass hair transplant’ – a six-year perspective. Hair Transplant Forum Intl 2003; 12(1):176-178, 194-196.
34. Arnold J: Mini-blades and a mini-blade handle for hair transplantation. Am J Cosm Surg 1997; 14(2):195-200.
35. Bernstein RM, Rassman WR: Limiting epinephrine in large hair transplant sessions. Hair Transplant Forum Intl 2000; 10(2):39-42.
36. Hasson V. The coronal incision recipient site Unger WP, Shapiro R. Hair transplantation. New York: Marcel Dekker; 2004. 898-900.
37. Martinick JH. Coronal (CAG) versus sagittal angled grafting (SAG). Hair Transplant Forum Intl 2003; 13(2):293-296.
38. Parsley WM. Coronal vs. sagittal recipient incisions. ESHRS Journal; Winter 2003:14-15.
39. Bernstein RM, Rassman WR, Rashid N, Shiell R: The art of repair in surgical hair restoration – part I: basic repair strategies. Dermatol Surg 2002; 28(9):783-794.
40. Bernstein RM, Rassman WR, Rashid N, Shiell R: The art of repair in surgical hair restoration – part II: the tactics of repair. Dermatol Surg 2002; 28(10):873-893.






