Robert M. Bernstein, MD*, New York, NY and William R. Rassman, MD, Los Angeles, CA
Dermatologic Clinics 2005; 23(3): 393-414. Issue on Advanced Cosmetic Surgery © 2005 by Elsevier Inc.
* Associate Clinical Professor of Dermatology, College of Physicians and Surgeons, Columbia University, New York, NY
INTRODUCTION
Follicular Unit Transplantation has its origins in the single-strip harvesting and stereo-microscopic dissection techniques of Dr. Bobby Limmer. He began using these hair restoration techniques in his own practice in 1988 and published them in “Elliptical Donor Stereoscopically Assisted Micrografting as an Approach to Further Refinement in Hair Transplantation” in 1994.1 The term “follicular unit” and the conceptual framework for Follicular Unit Transplantation were introduced into the medical literature by Bernstein and Rassman in the 1995 paper “Follicular Transplantation”2 and detailed in the paired articles, “Follicular Transplantation: Patient Evaluation and Surgical Planning” and “The Aesthetics of Follicular Transplantation” (1997).3,4
Follicular units are the naturally occurring groups of one to four terminal hairs that are present in a person’s scalp. Each group also contains sebaceous glands, a neurovascular plexus, an erector pilorum muscle and occasional vellus hairs and is surrounded by a circumferential band of adventitial collagen, the perifolliculum.5 The essence of Follicular Unit Transplantation (FUT) is to use these individual, follicular units exclusively in the hair restoration process.2
The concepts central to Follicular Unit Transplantation have been detailed in a previous issue of Dermatology Clinics and readers are encouraged to refer to that publication.6 Follicular Unit Transplantation has now become the standard technique used for hair transplants. According to an annual survey conducted in September 2003 by the International Society of Hair Restoration Surgery, 94% of the 121 members polled said they use follicular unit grafts. Only 15% reported using the traditional plug grafts.7 It is of note, however, that despite the widespread adoption of the technique, some of the core ideas of FUT are still being actively debated.8 The key concepts of Follicular Unit Transplantation6 are:
1) The follicular unit is a discrete anatomic/physiologic entity
If one considers the follicular unit as a distinct anatomic and physiologic entity, then preserving the follicular unit during dissection is the logical way to ensure the naturalness of the hair transplant and maximize hair growth. The advantage of follicular units over other grafting techniques in insuring a totally natural result has been the main reason for its widespread acceptance. However, the question of whether using these units exclusively will insure maximum yield is still subject to debate.9,10
It is not clear if single hair follicles, carefully dissected and placed into the recipient site, will grow as well as intact follicular units. However, from a practical standpoint, dividing follicular units increases the risk of follicular transection, with the divided units being more subject to desiccation, warming and crush injury during graft placement.11,12 Since intact units will already produce a natural result, it is hard to make a case for their sub-division. The rare exceptions would be in eyebrow transplantation (since the eyebrows consist of all 1-hair follicular units) and in very small procedures where there are not enough 1-hair units to complete the hairline. It could be argued that using grafts larger than follicular units could potentially decrease the risk of injury, but this creates a less natural appearance and greater recipient wounding – a poor trade-off when dissection injury can be minimized by careful stereo-microscopic dissection.
2) Only individual follicular units should be used in the surgical hair restoration procedure
Follicular units are relatively compact structures, but are surrounded by substantial amounts of non-hair bearing skin. The actual proportion of non-hair bearing skin is approximately 50%, so that its inclusion in the dissection will have a substantial effect upon the outcome of the hair transplant surgery.13 When multiple follicular units are used (with the intervening skin included) these effects will be magnified. (Figure 1.)
The advantage of using individual follicular units is that the wound size can be kept to a minimum while the amount of hair that can be placed into it can be maximized. Having the flexibility to place up to 4 hairs in a tiny recipient site has important implications for wound healing, the transplant design, and the overall cosmetic impact of the surgery.
3) Recipient sites should be kept as small as possible
Large incisions cause more damage to the cutaneous vasculature than small wounds and, although the blood supply of the scalp is extensively collateralized, damage to these vessels may still adversely affect local tissue perfusion. This becomes more significant when transplanting grafts in large quantities or when there are structural changes in the underlying connective tissue (i.e. that caused by ultraviolet radiation). Another advantage of small wounds is creating a “snug fit.”
Unlike a punch, which removes recipient connective tissue, a small needle-made incision, retains the basic elasticity of the recipient site. When a properly fitted graft is inserted, the recipient site will then hold it snugly in place. This “snug fit” has several advantages. During surgery, it minimizes popping, and the need for potentially traumatic graft reinsertion. After the procedure, it ensures maximum contact of the implant with the surrounding tissue, so that oxygenation can be quickly re-established. In addition, eliminating dead space minimizes the coagulum that forms around the graft and this, in turn, facilitates wound healing.
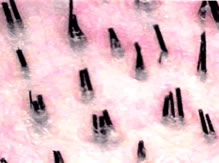 Figure 1. Normal scalp. Densitometry showing natural hair groupings (the surface manifestations of follicular units) in an area of where the hair is clipped to 1-mm. Two discrete populations of hair can be seen; larger terminal hair and scattered fine vellus hair.
Figure 1. Normal scalp. Densitometry showing natural hair groupings (the surface manifestations of follicular units) in an area of where the hair is clipped to 1-mm. Two discrete populations of hair can be seen; larger terminal hair and scattered fine vellus hair.Large wounds cause cosmetic problems that include dimpling, pigmentary alteration, depression or elevation of the grafts, or a thinned, atrophic look. The key to a natural appearing hair transplant is to have the hair emerge from perfectly normal skin. The only way to ensure this is to keep the recipient wounds small.
4) Follicular units should be transplanted in large sessions
There are several reasons to transplant large numbers of grafts in each session:
Social issues – large sessions allow the hair restoration to be completed as quickly as possible and allow the patient to appear normal during the process, since the whole area to be transplanted can be covered in each session.
Planning for Telogen effluvium – an inevitable aspect of hair transplant surgery is that the patient’s existing hair in and around the transplanted area has a chance of being shed as a result of the procedure. The hair that is at greatest risk of being lost is the hair that has already begun the process of miniaturization and, if this hair is at or near the end of its normal life span, it may not return. One should transplant through (rather than around) an area that is highly miniaturized, since it is likely that this area will be lost by the time the hair transplant has grown in. One should also attempt to transplant enough follicular units so that the volume of transplanted hair is greater than the volume of hair that may be permanently lost after the shedding.
Economizing the donor supply – regardless of how impeccable the surgical technique, each time an incision is made in the donor area, and each time sutures are placed, hair follicles are damaged or destroyed. This damage can be minimized by a fewer total number of hair restoration sessions, by low wound tension, by keeping the sutures very close to the wound edges (so that they don’t incorporate much hair-bearing tissue) and, in subsequent procedures, using the previous scar as the upper or lower boarder of the new excision.
Enhancing the composition of follicular units – in FUT, each graft represents one follicular unit. It follows that if we are to use only the naturally occurring individual units of 1 to 4 hairs, we are limited by their normal distribution in the scalp. With larger sessions, greater numbers of each type of unit will be generated and this will ensure that there will be enough 1-hair grafts to create the soft transition zone of the frontal hairline (without splitting units) and a sufficient number three- and four-hair grafts will be available to give the patient a full, rather than diffusely thin look.
5) Follicular units have a relatively constant distribution in the scalp of 1 unit per mm2
The relative constancy of the follicular unit density at 1/mm2 has been observed after performing densitometry measurements on thousands of patients and has been observed histologically by Headington as early as 1982.2,5 Although the follicular unit density is not exactly 1/mm2 , it is close enough to this number in most Caucasian scalps that it can be useful in the surgical planning. It is significantly less in the dark skinned races and will decrease in everyone’s scalp as one moves laterally from the densest part over the occiput, towards the temples. However, it explains the general observation that as hair density increases there will be more hairs per follicular unit rather than follicular units spaced more closely together.
The implication is that the same number of follicular units should generally be used to cover a specific size bald area regardless of the hair density of the patient. Transplanting a patient with low hair density, using the same number and spacing of follicular units as in a patient with high density, will help to ensure that there is proper conservation of donor hair for the long-term, even though the results will appear less full. If we try to give the patient with low density a “thick” look by combining units, one risks running out of donor hair.
6) Strip Harvesting should be performed in single, rather than multiple strips
Hair not only grows at an acute angle, but this angle varies in different parts of the scalp and in adjacent areas. Since the harvesting phase of the hair transplant surgery is relatively “blind” and doesn’t allow for complete control of these variations, single strip harvesting will minimize follicular transection, as it removes tissue with the minimum amount of cut surface area. Once the strip is harvested, stereo-microscopic dissection will prevent damage to the hair-bearing structures.
Follicular units can also be removed by direct extraction from the donor area using small punches, in a procedure called Follicular Unit Extraction (FUE). Although, this surgical hair restoration procedure is gaining popularity from its ability to avoid a linear donor scar, it has the dual disadvantages of being a relatively blind technique (so that there is a greater rate of transection) and of causing greater wounding than single-strip harvesting (in terms of absolute surface area).14,15
7) All dissection should be performed under stereo-microscopic control
In order to keep follicular units intact and dissect them without damage, visibility is the key. Only stereo-microscope dissection allows their clear visualization in both normal and scarred skin, independent of the specific hair characteristics of color, hair shaft diameter, and curl.
PATIENT SELECTION
In men, androgenetic alopecia is diagnosed by the characteristic “patterned” distribution of hair loss and by the presence of miniaturization in the areas of thinning. A family history of hair loss is supportive, but not necessary, for the diagnosis.16 In women, the diagnosis is more difficult, since the most common presentation, a diffuse pattern, can be mimicked by a number of other medical conditions. The presence of miniaturized hair will aid in the diagnosis, but it is important to rule out non-androgenetic etiologies. Miniaturization, the progressive diminution of hair shaft diameter and length, in response to systemic androgens, is easily observed using a densitometer, a hand-held instrument that magnifies a small area of clipped scalp. (Figures 1, 2)
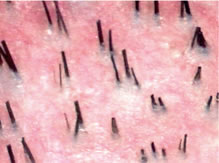 Figure 2. Miniaturization. Thick terminal hair, fine vellus hair, and hair of intermediate diameter (miniaturized hair) caused by the effects of systemic androgens on susceptible follicles.
Figure 2. Miniaturization. Thick terminal hair, fine vellus hair, and hair of intermediate diameter (miniaturized hair) caused by the effects of systemic androgens on susceptible follicles.The most widely used classification of male pattern hair loss is the one developed by Norwood.17 In the common pattern, two areas of hair loss, a bitemporal recession and a thinning crown, enlarge and eventually coalesce to form a large bald area that covers the entire front, top and crown (vertex) of the scalp. (Figure 3) In the Type A Variant, there is an anterior to posterior progression of the hair loss. (Figure 4) Although the sides and back tend to resist androgenetic changes, these areas may exhibit significant thinning in advanced age.
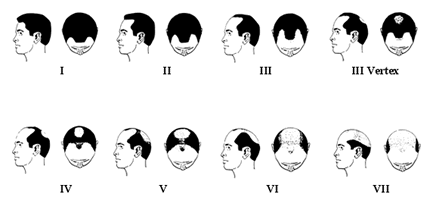 Figure 3. Norwood Classification – Common Type
Figure 3. Norwood Classification – Common Type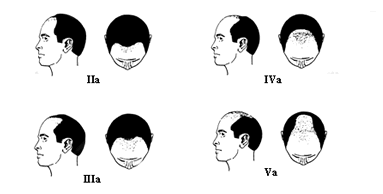 Figure 4. Norwood Classification – Type A Variant
Figure 4. Norwood Classification – Type A VariantTwo other, less common types of genetic hair loss are, Diffuse Patterned Alopecia (DPA) and Diffuse Unpatterned Alopecia (DUPA) which manifest as diffuse thinning in the front, top and vertex. As with female pattern hair loss, these may mimic other conditions and pose both diagnostic and therapeutic challenges. It is important to distinguish between DPA (which has a stable donor area) and the less common DUPA (where the donor fringe continues to thin significantly over time), since patients with DUPA are not candidates for surgical hair restoration.
DUPA tends to advance faster than DPA and eventuate in a horseshoe pattern resembling the Norwood class VII. However, unlike the Norwood VII, the DUPA horseshoe can look almost transparent due to the low density of the back and sides.3 The early signs of DUPA are: 1) a rapid decrease in hair volume (as distinguished from density) and a change in hair texture at an early age (often in the teens), 2) the maintenance of an adolescent hair pattern and persistent frontal hairline in spite of dramatic volume change, 3) a see-through donor area, which is greatly accentuated when the hair is lifted up, 4) significant miniaturization of the donor area (>35%), and 5) a donor density < 1.5 hairs/mm2.
If a diagnosis of DUPA is suspected, any decisions regarding hair transplant surgery should be postponed. The chance of missing the diagnosis of diffuse patterned alopecia argues strongly against performing hair transplantation at an early age.18
Although there are exceptions, it is generally best to wait until a person is 25 before considering surgical hair restoration. With the availability of effective medications for hair loss (finasteride and minoxidil) delaying surgery has become somewhat easier, since, in addition to growing or maintaining hair, they can be used to temporize the patient until hair transplantation is indicated. Barring untoward reactions, finasteride should always be used at least one year before judging its effectiveness. The patient should be warned that during the first 6 months, hair loss may be accelerated from these medications.
There are several important reasons not to perform surgery when a person is too young. First, the extent and rate of hair loss is more difficult to predict. Second, as discussed above, a diagnosis of DUPA may be missed. Third, the younger patient commonly wants his adolescent hairline and density restored. Restoring the hairline to its original position will look unnatural as the patient ages. Restoring a patient’s original density, of course, is not a realistic goal of a hair transplant, which services only to redistribute existing hair. By the time a patient reaches his mid-20’s he is more likely to be forward-looking and have expectations that can be satisfied with surgery.
Hair and Scalp Characteristics
When assessing a patient with androgenetic alopecia, one generally focuses on the extent of balding, i.e. matching the patient’s hair loss to a particular class on the Norwood scale and then anticipating how far he might progress considering his age, rate of hair loss, family history and use of medications. Possibly a more important consideration, however, is the patient’s donor supply. If one assumes that balding is progressive and that the ultimate degree of hair loss in unknowable, then one should only treat patients who possess enough donor hair to complete the hair restoration in the event of extensive baldness. This would be particularly important when the patient has not yet reached middle age and the predictive powers of the physician are the weakest.
Three major factors determine a patient’s donor supply; donor density, scalp laxity, and the physical size of the donor area. Hair characteristics, such as color, wave, and hair shaft diameter, also play a significant role, since a patient with good hair characteristics will obtain more coverage and a fuller appearance for the same absolute number of hairs transplanted, than someone with hair qualities that are less ideal. Light hair color, a wide hair shaft diameter and curly or wavy hair are attributes that will make the hair transplant look fuller.
The average Caucasian has approximately 175-275 hairs/cm2 (approximately 80-120 follicular units/cm2).8 For patients with average density and average hair characteristics, approximately half of the hair in the donor area may be moved without it appearing too thin. This will also provide enough coverage to camouflage the donor scar. Therefore, hair may be harvested from the donor area until the density approaches 100 hair/cm2.2 As a general guide, virgin scalp should have a donor density of at least 150-180 hairs/cm2 for surgical hair restoration to be considered, with the lower end of the range being reserved for the older patient or those with excellent hair characteristics. In non-Caucasians, the normal density is less, so the lower limit can also be adjusted downward.4 To be a candidate for surgery, no more than 20% of the hair in the donor area should exhibit miniaturization.
Scalp laxity is another important factor in determining total available donor supply. Although difficult to quantify, a significantly greater amount of hair can be harvested from persons with loose scalps compared to those whose scalps are tight. The limitations of a tight scalp usually manifest itself after the first procedure so assessing scalp laxity at the outset can be difficult. Nevertheless, its assessment can not be over emphasized, since patients with tight scalps can have a very limited donor supply and their long-term goals must be accordingly reduced.
Interestingly, hair transplant patients with very loose scalps tend to heal with widened scars and this will also limit the amount of transplantable donor hair.19 Follicular unit extraction (FUE), a harvesting method that does not require a linear donor incision, should be considered in cases of very loose and very tight scalps. Sometimes, however, FUE is difficult to perform in patients whose scalps are very loose.14
Finally, the physical dimensions of the donor area will affect the amount of transplantable hair. The mid-portion of the harvestable donor zone is generally at the level of the occipital protuberance and extends to within 3cm of the temple hairline on either side, a distance of approximately 33cm. It is important to keep the incision at this level, since an incision that is too high risks harvesting hair that may not be permanent and an incision that is too low increases the chance of a widened scar.
Pages:






