Schedule Your Consultation
HAIR LOSS
SOLUTIONS
HAIR LOSS
SOLUTIONS
Let the team at Bernstein Medical
Find the best option for you.
- Before & After Photos
- Photo Journal
- FAQ
- FUE vs FUT
- Answers
- Video
- Physician Consult
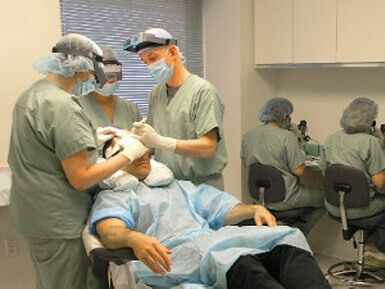
Hair transplantation is an out-patient surgical procedure in which hair is transplanted from the back and/or sides of the scalp (the “donor area”) to areas that are thinning or bald (the “recipient area”). Once transplanted, the hair will generally grow for a person’s lifetime. In addition to treating androgenetic alopecia (common genetic hair loss), surgical techniques can be employed to restore eyebrows, facial hair, and pubic hair, and to repair scars caused by trauma or surgical procedures such as face-lifts and prior surgeries.
All modern hair restoration surgeries are based on a concept introduced by Dr. Bernstein in his groundbreaking 1995 publication “Follicular Transplantation.” In this, and in a series of papers that followed, he proposed that the most aesthetically pleasing outcomes will be produced when individual naturally-occurring bundles of one to four hairs, called follicular units, are transplanted rather than the larger grafts of skin and hair used in traditional procedures. These publications laid the groundwork for modern surgical hair restoration.
Christine M. Shaver
Medical Director
-
 Board-certified dermatologist
Board-certified dermatologist -
 Mohs micrographic surgeon
Mohs micrographic surgeon -
 M.I.T., Yale University
M.I.T., Yale University -
 Alpha Omega Alpha (AOA) honors
Alpha Omega Alpha (AOA) honors -
 FUT and Robotic FUE
FUT and Robotic FUE

Before and After Hair Transplant
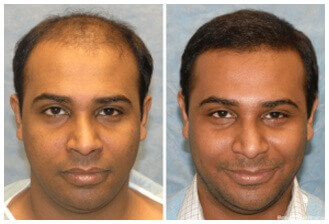
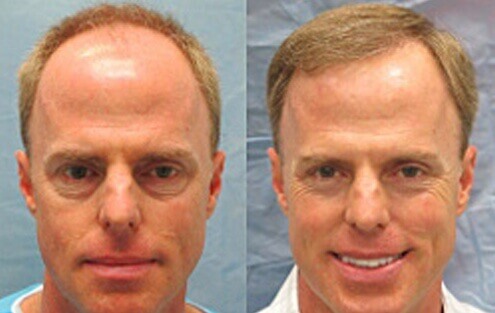

Types of Procedures
Follicular Unit Transplantation (FUT)
Dr. Bernstein’s breakthrough idea of transplanting only naturally occurring follicular units led him to develop a procedure called Follicular Unit Transplantation (FUT). FUT became the gold standard in surgical hair restoration and is still performed around the world. In FUT, the patient’s scalp is numbed using local anesthesia, and a strip of skin is removed from the donor area. This “donor strip” is subsequently dissected with the aid of special stereo-microscopes into hundreds or thousands of grafts, each of which contains an individual follicular unit. The donor area is sutured or stapled closed to produce a very fine linear scar.
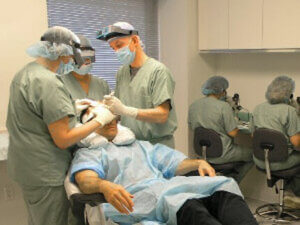
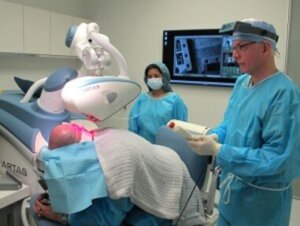
Follicular Unit Extraction (FUE) & Robotic FUE
Dr. Bernstein pioneered Follicular Unit Extraction (FUE) in 2002 (with his colleague Dr. William Rassman) and robotic-assisted FUE (Robotic FUE) in 2011. In FUE, follicular units are removed one-by-one directly from the donor area using a small, round cutting instrument. As with FUT, the grafts are then implanted one-by-one into recipient sites in the balding scalp. The small holes that remain from the extraction are left open to heal, which takes about a week, with each producing a tiny, round, white scar. There are a variety of manual and motorized instruments for FUE, including the Neograft and the SAFE System.
Candidacy for Surgery
Surgical hair restoration should only be performed on appropriate candidates. This assessment occurs during a hair loss consultation with a physician. In order to be a candidate, five basic criteria should be met. These include:
- A diagnosis of androgenetic alopecia (common genetic hair loss) or another condition that is amenable to surgical hair restoration
- First explored medical therapy and, if appropriate, given adequate time to see a full response (generally one year)
- Sufficient hair loss that it affects their aesthetic appearance
- Adequate donor hair to satisfy current and future needs
- Realistic expectations on what surgical hair restoration can accomplish
What Age to Consider Surgical Hair Restoration
Young patients should not consider surgery as a technique to prevent hair loss, as it does not block the hormones that cause genetic balding. Rather, hair surgery is a restorative treatment to improve your appearance if other modalities have been unsuccessful or can’t be used.
Candidacy in Women
With female patients, it is important for the physician to ensure that the patient’s donor area is stable and not prone to thinning. Comprehensive diagnostic testing is often required to rule out underlying medical conditions, medication, or pregnancy as the cause of the hair loss; confirm the diagnosis of androgenetic alopecia, and determine if the patient is a candidate for surgery.
Consultation for Surgical Hair Restoration
Every patient at Bernstein Medical must have a one-on-one consultation with a board-certified hair restoration physician to determine if they are a candidate for a hair transplant. At the consultation, the doctor will listen to the patient’s concerns regarding their hair loss, take a careful medical history, and ask about their expectations for the hair restoration. The patient will have plenty of opportunity in the consult to ask questions about their hair loss and how best to treat it.
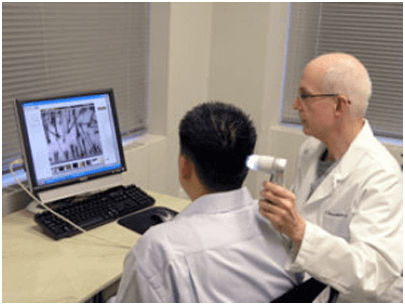
Densitometry & Miniaturization
Dr. Bernstein’s breakthrough idea of transplanting only naturally occurring follicular units led him to develop a procedure called Follicular Unit Transplantation (FUT). FUT became the gold standard in surgical hair restoration and is still performed around the world. In FUT, the patient’s scalp is numbed using local anesthesia, and a strip of skin is removed from the donor area. This “donor strip” is subsequently dissected with the aid of special stereo-microscopes into hundreds or thousands of grafts, each of which contains an individual follicular unit. The donor area is sutured or stapled closed to produce a very fine linear scar.
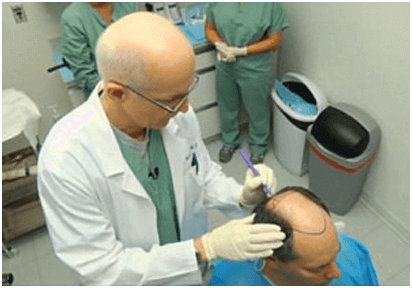
Design & Planning
During the consult, the physician will begin to make the necessary aesthetic judgments to formulate the design. These judgments include how best to distribute a finite amount of donor hair for maximum cosmetic effect, how to design the hairline, and how to restore the crown (when appropriate). The transplant design should be made in collaboration with the patient’s needs, but the plan must be a realistic one, taking into account future hair loss and the fact that everyone’s donor supply is finite.
The Procedure
Hair transplantation is a minimally-invasive surgical procedure performed under local anesthesia in the doctor’s office or outpatient facility. A typical session entails the extraction and placement of 300 to 3,000 follicular unit grafts. Procedures can last eight hours or more and the longest ones are performed over two consecutive days. How long the procedure takes depends on the number of follicular units transplanted and the type of procedure used, with FUE generally taking longer than FUT.
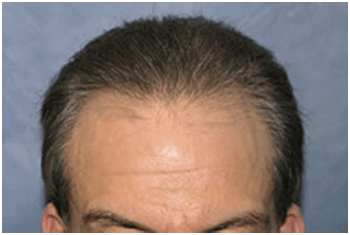
Post-op Growth
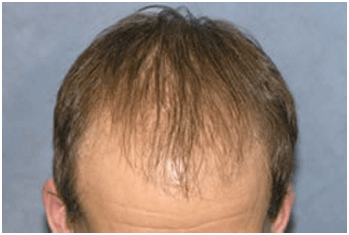

Other Applications for Surgical Hair Restoration
Repair Procedures
Surgical hair restoration techniques can be used to correct the appearance of poorly executed transplants, old “hair plug” procedures, scalp reductions, flaps, or widened donor scars. In camouflage procedures, follicular units are implanted around the plugs or scars to hide them. In a graft excision, large pluggy grafts — which can contain several follicular units — are removed and dissected into individual follicular units. These are re-implanted into balding areas, turning a row of unnatural-looking plugs into a more natural hairline. In “combined repair” procedures, both of these techniques are used to achieve the most natural look. Many patients in need of repair procedures have very limited donor hair reserves, so each step in the repair process must be performed with extreme care. Read about corrective methods, and the situations in which each would apply, in the Repairs section.
Eyebrow Transplant & Restoration
The specific anatomic features of eyebrows require special techniques to create natural-looking results in this cosmetically most important area. Fortunately, due to the limited amount of hair needed in eyebrow restoration, most patients will have adequate donor hair if they are candidates for the procedure. Read more in the Eyebrow Transplant & Restoration section.

Hair Restoration History
- The first surgery for male pattern baldness was performed by Dr. Norman Orentreich in 1952 in New York City. He formally introduced surgical hair restoration in his 1959 publication, “Autografts in alopecias and other selected dermatological conditions.”
- From the 1960s through the early-80s, Orentreich’s procedure used 3-4mm grafts that became known as “hair plugs.”
- In 1984, it was first proposed to use smaller grafts (mini-grafts) cut from a strip of tissue taken from the donor area. Physicians began using “micro-grafts” of one to two hairs to soften the frontal hairline, and by the 1990s use of “mini-micro graft” techniques resulted in a phasing out of the “plug” procedures.
- In 1995, Dr. Bernstein introduced the idea of transplanting exclusively naturally-occurring follicular units in his landmark paper, “Follicular Transplantation.” Since then, all modern hair restoration surgeries have been based on this concept.
- By 2000, Follicular Unit Transplantation (FUT) had become the “gold standard” technique for thousands of patients worldwide.
- Along with his colleague, Dr. William Rassman, Dr. Bernstein introduced Follicular Unit Extraction (FUE) to the medical literature in a 2002 publication titled “Follicular Unit Extraction: Minimally Invasive Surgery for Hair Transplantation”.
- In 2004, Dr. James Harris introduced a two-step sharp/dull punch instrument for FUE which is important in minimizing damage to the follicular units during extraction.
- In 2011, Restoration Robotics, Inc., introduced the ARTAS Robotic System, the first and only robot for use in FUE. In the fall of 2011, Bernstein Medical became one of the first hair restoration facilities in the world to perform Robotic FUE using the ARTAS Robot. The robot uses the two-step sharp/dull punch tool.
- Since 2011, Dr. Bernstein has collaborated with Restoration Robotics to improve the robot’s performance and develop other applications of the robot. Bernstein Medical is a beta-testing site for Restoration Robotics, and it was in our New York City facility where Dr. Bernstein débuted robotic recipient site creation and automated follicular unit graft selection, along with many other hardware and software upgrades.