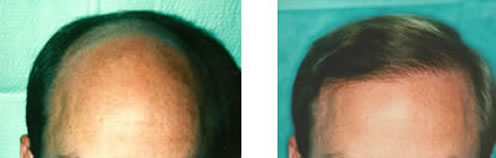
Charles Gibson: In a two-part series this week, “The Bald Facts,” we are looking at what works and what doesn’t in hair replacement.
And first up, we want you to meet Charles Teacher, a real estate executive who for 30 years has been a guinea pig for every kind of baldness remedy there was. Let’s look at his struggle through the years.
Charles Teacher: It was very restrictive. You’re always patting it down, looking in the mirror to see that it’s not sort of showing. It’s a really difficult way to live.
Charles Gibson: Charles Teacher should know. He’s been studying the latest trends in baldness for three decades. His hair started thinning when he was just 26, and back then he tried that bastion of hope, the comb-over.
Charles Teacher: I still had hair then. You couldn’t see that I was bald, but I could see I was very thin. It really is this fear of being unattractive to women. I suppose it is a certain amount of vanity in terms of how you look, but most of it is this fear of being rejected.
Charles Gibson: So even at an early age, he began wearing a toupee and bemoaning his genetic fate. His father had male pattern baldness. Would he spend the rest of his life worrying which way the wind blew on the golf course? Then came 1977 and the heralding of the hair plug. Charles Teacher was first in line for the surgery, and what a surgery it turned out to be.
Charles Teacher: Most of the plugs didn’t take and the few that did were in the front in a very bad hairline. It looked stupid.
Charles Gibson: This was the hairline of those old plugs, right across his forehead, so he went back to his toupee. He had a curly rug when styles were curly, a grayer one as he grayed, and he wore his hairpiece to bed. Even his wife never saw him without it.
Charles Teacher: She never saw me without the hairpiece for 30 years until I had the consultation with the surgeon who is doing the transplant and I removed it off like that.
Charles Gibson: The consultation was with hair transplant surgeon Robert Bernstein who recommended Teacher go bald, just a better bald, moving hair around to give him more on top. He demonstrated with before and after pictures of former patients. Teacher signed on and had the old plugs removed which would be added on with the rest.
Years ago in transplants like Charles Teacher’s, the surgeon removed small circles of tissue from the back of the head where hair growth is stable, then to transplant those clumps of up to 30 hairs, the surgeon would remove a matching circle of tissue from the top of the head and put in the graft. It worked, but it didn’t look natural.
Dr. Bernstein: That has always been the problem, that grafts that were done 25, 30 years ago are still around. So really the idea is not just to get the hair to grow. That’s the simple part. The challenge is to do it in a way that looks natural.
Charles Gibson: Now Charles Teacher’s best hope, single follicular unit transplants. The surgeon removes a strip of hair-producing tissue from the back of the head and separates it under a microscope into units of one to four hairs, the way hair grows naturally. The surgeon then makes tiny incisions exactly where and at what angle he wants each hair to grow and then implants it.
Teacher decided it was worth a try, even though it would cost thousands of dollars. Now he wants to burn his old toupee for one of the best results of all, to go swimming with his new grandchild, carefree.
Charles Teacher: I really feel that I’ve been given a new lease in life in many ways. It sounds silly, but just to be normal, just to be normal.
Charles Gibson: We’re joined by Charles Teacher, sans toupee, and the man who helped to get rid of it, Dr. Robert Bernstein, Associate Clinical Professor of Dermatology at Columbia University.
Good to have you both here. Why go through all this trouble? Why not just be bald?
Charles Teacher: I think it’s because I started with a hairpiece when I was rather young, 26, and I just didn’t have the guts to take it off. I think I felt a bit like Samson and Delilah, should we say, you know, if I lost my hair, I’d lose my strength or my personality.
Charles Gibson: And you’re pleased with this.
Charles Teacher: It’s just awesome.
Charles Gibson: Dr. Bernstein, is his hair actually growing? I had always heard that you can transplant hair, but you can’t make it grow.
Dr. Bernstein: No, actually, a transplant will continue to grow. He has to get haircuts just like it’s his normal hair.
Charles Gibson: Are there good candidates and bad candidates for this?
Dr. Bernstein: Yes. And actually people that wear hairpieces are sometimes tricky because their baseline is a full head of hair, so one of the important things that we had to discuss in the first consult was what his expectations were and whether he realized that a transplant wouldn’t give him the fullness of a hairpiece, but of course, it would look much more natural.
Charles Gibson: That’s why you lose the line, you’re still bald to some extent, but it’s a better kind of bald.
Dr. Bernstein: Yes.
Charles Gibson: Single follicular unit transplants is such a mouthful, but basically it’s saying you’re just transplanting a hair two or three at a time.
Dr. Bernstein: Right. In the old days, hair was planted in little clumps and then it was divided into small pieces but arbitrarily. Now we transplant hair exactly the way it grows in nature, and hair normally grows in little tiny bundles and they’re called follicular units.
Charles Gibson: I don’t know if it’s dirty trick, but we have a camera behind you because in the back of your head, you’re going to have a second procedure now.
Charles Teacher: Yes, we’ll have a second procedure actually this morning. I think that we’ll leave the back and probably just reinforce the front so that it –- I mean, you don’t really see the back of your head, you’re only worried about how you appear in the mirror.
Charles Gibson: Right. How much does it cost?
Charles Teacher: I haven’t told my wife. Can I give that a miss?
Charles Gibson: Well, I’m sure Dr. Bernstein, he’ll probably say something.
Dr. Bernstein: We charge about $5 a graft.
Charles Gibson: About $5 a graft, which is one, two, three, four, five hairs –-
Dr. Bernstein: That’s right.
Charles Gibson: — per time. So that gets rather expensive. I mean, we’re talking about $10,000, $15,000 for a total procedure?
Dr. Bernstein: Yes.
Charles Gibson: Which insurance does or does not cover?
Dr. Bernstein: It usually does not.
Charles Gibson: But you probably spent that much in toupees over the time.
Charles Teacher: Absolutely. You know, so $2,000 or $3,000 a year with the toupees and the hairdresser worrying every week, you know, yeah.
Charles Gibson: Gotta ask. You’re a little thin on top yourself, yet you haven’t done this.
Dr. Bernstein: Everybody asks me that. It just doesn’t bother me. And I think it’s important being a doctor that people, when they come to see me, they don’t feel compelled that they have to have the transplant, that they’re here because they want to. And that being bald is okay.
Charles Gibson: So the title, if somebody’s interested in this, is follicular unit transplant.
Dr. Bernstein: Yes.
Charles Gibson: All right. Dr. Bernstein, thanks very much. Charles Teacher, thank you very much.
Charles Teacher: Thank you.
Charles Gibson: Good to see you. Good luck with the procedure today.
Charles Teacher: Thank you.




 “Hair doesn’t grow singly it grows in naturally occurring groups of from one to four hairs. In follicular transplantation, we use these naturally occurring groups as the unit of the transplant,” he told CST.
“Hair doesn’t grow singly it grows in naturally occurring groups of from one to four hairs. In follicular transplantation, we use these naturally occurring groups as the unit of the transplant,” he told CST.