Viviscal May Boost Hair Regrowth
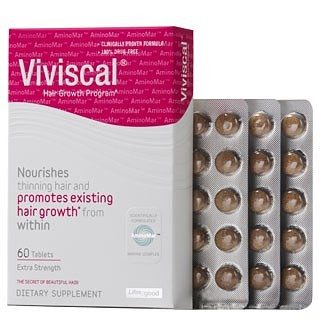
A study published in the December 2015 issue of the Journal of Clinical and Aesthetic Dermatology suggests that Viviscal, an oral supplement designed for women with thinning hair, may promote hair growth. The researchers noted a 79 percent increase in healthy, terminal hairs and an almost 12 percent increase in hair diameter in female patients who took the supplement for six months. The evidence suggests that Viviscal may be a useful supplement to current hair restoration treatments, or an alternative treatment in patients not indicated for hair transplant surgery or medical treatment with finasteride.
Viviscal May Boost Hair Regrowth Read More »


 Topical application of the solution containing melatonin, ginkgo biloba and biotin was found to reduce hair loss, and in some cases grow new hair. Incidence of seborrhea was also reduced by the treatment. While the exact mechanism for this result is unknown, if effective, it is likely related to the antioxidative effect of melatonin and/or a melatonin receptor-mediated antiandrogenic effects. More research on melatonin needs to be conducted, but this study acts as a proof of concept for the use of melatonin as a treatment for early hair loss in men and women and potentially as a treatment for seborrhea.
Topical application of the solution containing melatonin, ginkgo biloba and biotin was found to reduce hair loss, and in some cases grow new hair. Incidence of seborrhea was also reduced by the treatment. While the exact mechanism for this result is unknown, if effective, it is likely related to the antioxidative effect of melatonin and/or a melatonin receptor-mediated antiandrogenic effects. More research on melatonin needs to be conducted, but this study acts as a proof of concept for the use of melatonin as a treatment for early hair loss in men and women and potentially as a treatment for seborrhea.
 A double-blind scientific study published in the May 2012 issue of the Journal of the American Academy of Dermatology has found that latanoprost, a drug that mimics naturally-derived compound molecules called prostaglandins, significantly increases hair density on the scalp after 24 weeks of treatment in young
A double-blind scientific study published in the May 2012 issue of the Journal of the American Academy of Dermatology has found that latanoprost, a drug that mimics naturally-derived compound molecules called prostaglandins, significantly increases hair density on the scalp after 24 weeks of treatment in young 



