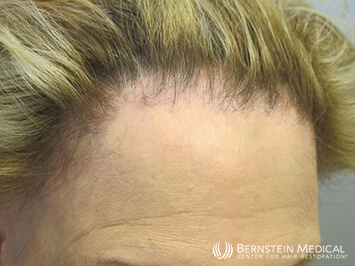
A 60-year-old woman presents with a 10-year history of hair loss at her frontal hairline. The area is occasionally itchy. She also notes some thinning and scaling of her eyebrows. She is otherwise healthy and does not take any medications. She denies tight hairstyles. There is no family history of hair loss. She last washed her hair 24 hours ago. A hair pull test is negative.
Q: What would be the next step?
- Laboratory bloodwork
- Trichoscopy of the scalp
- Biopsy of the frontal hairline
- Begin therapy with Platelet-rich plasma (PRP) and/or Rogaine (minoxidil)
Answer B. Trichoscopy of the scalp shows follicular hyperkeratosis and perifollicular erythema. There are scattered smooth scarred follicular ostia. There is a striking absence of miniaturized hair. Examination of the scalp with trichoscopy should precede biopsy as it is a non-invasive tool that provides information in real-time.
Q: What is the best next step?
- Scraping of the perifollicular scale with KOH microscopy
- Scalp Biopsy
- Minoxidil
- Trial of topical steroids
Answer B. Given the findings on trichoscopy, cicatricial alopecia is high on the differential. A biopsy should be performed to confirm the diagnoses of scarring alopecia.
Q: What is the best way to perform the biopsy?
- Punch biopsy an involved follicle including the fat and scarred tissue around it
- Try to incorporate as many involved hair follicles as possible into a punch that will comfortably fit without undue transection
- Biopsy a scarred area devoid of follicles
- Shave biopsy of several involved follicles
Answer A. Ideally, one should have at least one intact follicle with scarred tissue included. The primary cicatricial alopecias (LPP, FFA, follicular degeneration syndrome, CCCA) are all characterized by a lichenoid infiltrate in the region of the clinically involved follicles and loose fibrosis around the follicular remnants in the scarred areas. If there is no follicle, then connective tissue streamers may suggest a primary cicatricial alopecia, but this is less diagnostic. If a shave biopsy were deep enough to include intact follicles, there would be unnecessary scarring.
Q: What size punch should you use?
- 2mm
- 3mm
- 4mm
- 5mm
Answer B. To incorporate an entire follicle, the subcutaneous fat and follicular remnants, a minimum of 3mm to 3.5mm is needed. A smaller punch is more likely to not capture the entire follicle. Punches 4mm and greater will cause unnecessary scarring.
Q: Should the punch be perpendicular to the skin or parallel to hair follicles?
- Perpendicular
- Parallel
- It does not matter
Answer B. Aligning the punch parallel to the follicle will give the most information. It is important to observe the angle of exit of the hair from the scalp so that the punch can be aligned parallel to this angle and the entire follicle will be captured. If the punch is oriented perpendicular to the scalp, then the follicle will be transected underneath, and important diagnostic information will be lost.
Q: When performing the punch, should you:
- Stretch the skin along skin lines
- Stretch the skin perpendicular to skin lines
- Not stretch the skin
Answer B. If you stretch the skin perpendicular to skin lines, then the round punch incision will relax into an oval and make suturing easier. The suture should be placed perpendicular to the length of the oval (i.e., perpendicular to skin lines).
Q: How would you close the biopsy site?
- Skin glue
- 4-0 Nylon
- 5-0 Nylon
- Leave it open for second intention healing
Answer B. A 5-0 suture will often rip when trying to close an oval/circular incision into a line. In addition, the finer 5-0 suture may cut through the tissue if there is tension. For these reasons, a 4-0 suture is preferred. Skin glue will not hold the wound together. Second-intention healing will be slow to heal and leave an unnecessary scar. One, simple, interrupted suture is generally sufficient to close a defect from a 3mm punch biopsy. A 3.5mm punch may require two sutures. In all cases, a simple barrel stitch should be used to make sure the wound edges do not invert. For the best cosmetic scar, mild eversion should be attained so that, as the scar contracts during healing, the scar will flatten.
Q: What type of evaluation should you request on the biopsy you send to the laboratory?
- Direct Immunofluorescence
- Regular H&E with vertical sectioning
- Regular H&E with horizontal sectioning
- Regular H&E with both horizontal and vertical sectioning
- Tissue culture of the biopsy
Answer B or D. If the main concern is ruling out scarring alopecia then vertical sectioning alone is generally adequate. However, combining both horizontal and vertical sectioning maximizes the diagnostic yield. In general, horizontal sections are helpful in diagnosing conditions where follicular ratios are important, such as telogen effluvium and androgenetic alopecia. Horizontal sections can show follicular count, density, and ratios. Vertical sections allow for visualization of the full thickness of the skin and hair shaft profile over its entire length which is helpful for evaluating interface changes, peribulbar inflammation and fibrosis.
Q: When should sutures be removed?
- 7 -10 days
- 10-14 days
Answer B. A round punch wound has memory and will tend to spring open, especially in scarred skin. Removing stitches too early will risk wound dehiscence and a poor cosmetic result. Sutures for a 3mm or 3.5mm scalp biopsy should be left in for 10-14 days. This will prevent dehiscence and will rarely leave stitch marks.
Q: What is the most likely diagnosis?
- Traction alopecia
- Frontal fibrosing alopecia
- Androgenetic alopecia
- Alopecia areata
Answer B. FFA is a scarring alopecia subtype seen in predominantly women. A common complaint is recession of the frontal hairline and temples with associated loss of eyebrows and can be accompanied by tingling or itch. There can also be follicular scale and erythema. There is often a dramatic absence of miniaturized hair (which would be expected in areas of androgenetic thinning). Some patients may also complain of loss of eyelashes, or loss of hair on their arms or legs.
Q: How would you treat this patient?
- Topical minoxidil (Rogaine)
- Platelet-rich plasma
- Anti-inflammatory medications (topical/oral/injectable)
- Finasteride
Answer C. (Anti-inflammatory medications). Once a biopsy confirms the diagnosis of FFA, the next step is to discuss treatment strategies. The first line will be medical management with oral medications such as hydroxychloroquine and doxycycline, topicals such as corticosteroids, and intralesional injection of steroids as well.
If you are experiencing gradual hair thinning, please contact our office for an appointment. Call 212-826-2400 or schedule a consult here.





