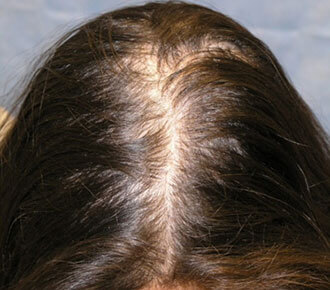
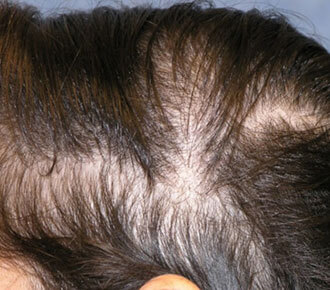
A 30-year-old woman presents with a 6-month history of recent hair loss. When asked whether she first noticed decreased hair volume (thinning) or more hair falling out (shedding) she thinks the latter is the main problem. She has no known medical problems and does not take any medicines. She denies recent weight loss, illness, new medications, or excessive stress. She has not had any recent bloodwork done, but regularly sees her doctor for wellness exams. She has regular periods with heavy flow. Her father has thinning across the top of his scalp and her maternal grandmother had diffusely thin hair. She last washed her hair 24 hours ago. On physical exam the patient’s hair looks thin but has an even distribution. An examination of the scalp is normal.
Q: What would be the next step(s)? Select all that would apply.
- Hair Pull
- Trichoscopy of the scalp
- Laboratory bloodwork
- Biopsy the scalp behind the frontal hairline
- Begin therapy with Platelet-rich plasma (PRP) or Rogaine (minoxidil)
Answer: A and B. A hair pull should be performed 24 hours after the last washing/brushing. A positive test suggests Telogen Effluvium. Trichoscopy of the scalp checks for miniaturization (i.e., variations in hair shaft diameter mainly caused by hair follicular susceptibility to DHT). This patient had a positive hair pull and normal miniaturization (<20%).
Q: What is the most likely diagnosis?
- Androgenetic alopecia
- Female Pattern hair loss
- Telogen effluvium
- Diffuse Un-patterned Alopecia (DUPA)
Answer: C. Telogen Effluvium. With a normal appearing scalp, no evidence of genetic thinning (miniaturization), and a positive hair pull test, the most likely diagnosis is telogen effluvium (TE).
Q: What would be the next step?
- Biopsy of the frontal hairline
- Laboratory bloodwork
- Retake the history
- Start PRP or Rogaine
Answer: C) Once a diagnosis of telogen is being considered a careful history is the key to diagnosis. This should include a complete systems review and careful drug, diet, social and family history.
Q: Which of the following blood tests should you order if the history is negative?
- A complete laboratory evaluation
- CBC, serum iron, serum ferritin, TFTs and sex hormone panel
- CBC, serum iron, serum ferritin, TFTs
- CBC, serum iron, serum ferritin
- An STS, ANA, Hep B, and Lyme titers
- No blood work is warranted at this time
Answer: C and D are both reasonable answers. Given the patient’s history of heavy menses, it would be reasonable to look for iron deficiency. Since thyroid disease is a common cause of hair loss, a screen for thyroid disease might uncover a subclinical cause of shedding. Male and female hormone panels would be more helpful with androgenetic hair loss, but unlikely to yield significant information in this case. Other blood work would unlikely offer any useful information with a negative history.
Q: What is the best therapy for TE?
- Rogaine
- Platelet-rich plasma
- Hair transplant
- Finasteride
- Reassurance
Answer: E) Reassurance. Telogen effluvium is a challenging diagnosis for patients to cope with since no treatment is available. Patients need to understand that the condition results from a ‘trauma’ that causes the hairs to shed excessively because many hairs enter the telogen (resting) phase simultaneously. This condition is reversible once the stressor has been managed but can take 1-2 years to resolve.
If you are experiencing gradual hair thinning, please contact our office for an appointment. Call 212-826-2400 or schedule a consult here.






