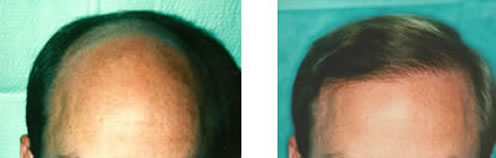
The highly-rated CBS television program “The Early Show” interviewed Dr. Bernstein as part of a three-part series on hair loss in women. View a clip of the video here:
Julie Chen: There are many treatments available for serious hair loss including surgical options like hair transplants. That may sound scary, but for one woman, it was the answer she’d been waiting for.
Narrator: Marian Malloy is used to being in control. As the duty manager for an international terminal at Newark Airport, it’s her job. But Marian wasn’t always so self-confident. Due to a condition called alopecia areata, Marian began losing her hair back in college.
Marian Malloy: I was on my own for the very first time and I was learning about life and learning about my hair loss. And it just devastated me. So I started out picking out methods to improve my hairline. Initially, I went to a dermatologists who put me on a prescription of injections, actually. I would go over weekly and he injected my head, and I got results, but I also started growing facial hair, which wasn’t something that I wanted. After that, I decided to start with the Rogaine and once again I saw results, but Rogaine was something that I had to do every day for the rest of my life, and I just didn’t want to be that dependent on a medication.
Narrator: Marian continued to search for an acceptable treatment to her condition, even trying hair plugs, until she heard about Dr. Robert Bernstein’s new method of Follicular Unit Transplantation, or in layman’s terms, a hair transplant.
Marian Malloy: I wasn’t scared at all. I was desperate, so that overrode everything.
Julie Chen: Marian Malloy is here along with her hair transplant surgeon, Dr. Robert Bernstein, to help us look at some of the medical options that are available to women suffering from this affliction.
Good morning to both of you.
Dr. Bernstein: Good morning.
Marian Malloy: Good morning.
Julie Chen: Marian, thank you for speaking out about this very private problem. How has your life changed since getting the hair transplant?
Marian Malloy: Well, I just feel better about my appearance, and appearance is very important to me in my line of work. I just feel a lot better and I think I look better. My hairline looks better.
Julie Chen: Boost in the self-confidence department?
Marian Malloy: Actually, yes.
Julie Chen: And your friends and family see a difference in it?
Marian Malloy: You know, my friends and family really didn’t notice a difference before, and they thought I was crazy for harping on it the way that I did.
Julie Chen: But if you see it, that’s all that —
Marian Malloy: And it was all about me. It’s not about my family and friends. It’s about how I feel.
Julie Chen: Right.
Marian Malloy: Yes.
Julie Chen: Dr. Bernstein, I want to go through all the options that are available for women, but what is the difference between female and male hair loss option-wise. What can we do to treat it?
Dr. Bernstein: The main difference medically is that women have hair loss often from hormonal changes and it’s due to an imbalance between progesterones and estrogens. That equilibrium can be reestablished with medication. Often birth control pills can do that.
Julie Chen: So that’s one option.
Dr. Bernstein: One option. For the most common cause of hair loss, genetic hair loss, Minoxidil can be used for both men and women, but the most effective medication for men, Propecia, can’t be used in women. And the reason –
Julie Chen: Why not?
Dr. Bernstein: The reason is that it causes birth defects if taken during pregnancy and postmenopausally it doesn’t seem to work.
Julie Chen: Oh, okay. So talk to me about Minoxidil, also known as Rogaine .Just as successful for women as in men?
Dr. Bernstein: It seems to be similarly successful, but the success rate is not very good, and one of the problems with its use in women is that you can get hair at the hairline on the forehead. So the usefulness is a little bit limited.
Julie Chen: So is it promoting hair growth if it does work, the Rogaine, or is it just making your existing hair grow in thicker? I’ve heard both.
Dr. Bernstein: It actually stimulates the growth of existing hair.
Julie Chen: Okay so you got to be really careful topically what you touch after you’re rubbing it into your scalp.
Dr. Bernstein: Yes.
Julie Chen: Another option is topical Cortisone and Cortisone injection.
Dr. Bernstein: Yes many people think that Cortisone can be used for genetic hair loss or common hair loss and it really can’t. It’s a good treatment for specific types of diseases, the most common one is alopecia areata. In that condition, the body actually fights off its own hair follicles. And then the Cortisone is used to suppress the immune system and actually allows the body to permit the hair to grow back.
Julie Chen: Now, Marian tried these options that we’re talking about. You weren’t satisfied, so you had a hair transplant.
Marian Malloy: Yes.
Julie Chen: Describe exactly what you did for Marian.
Dr. Bernstein: In the past, hair transplantation was not a good option for women because hair was transplanted in little clumps. With Follicular Unit Transplantation, we can now transplant hair exactly the way it grows, which is in little tiny bundles of one to four hairs. With Marian we took a strip from the back of her head, in other words, right from the back of the scalp where you can’t see it.
Julie Chen: Where there’s more hair?
Dr. Bernstein: Yes, we remove that strip and place it under a microscope and dissect out the individual follicular units – the hair is transplanted exactly the way it grows in nature. And that hair is then put in needle-poke incisions all along the hairline, and because the grafts are so small, you can actually mimic the swirls and the change in hair direction exactly the way the hair grows naturally.
Julie Chen: And it stays?
Dr. Bernstein: Yes, it stays. We make a very snug fit between the graft and the needle-poke incision. And so it really holds on to the grafts well. In fact, the patients can shower the next morning.
Julie Chen: The next morning? Marian, what was your experience like having this hair transplant? No problems since?
Marian Malloy: No problems, absolutely no problems.
Julie Chen: Did insurance cover any of this?
Marian Malloy: No, absolutely not.
Julie Chen: How costly is this?
Dr. Bernstein: The average procedure is about $7,000.
Julie Chen: And it’s one procedure and you’re done?
Dr. Bernstein: Usually one to two procedures.
Julie Chen: $7,000 a pop. Well, you found it was worth your money, is that right, Marian?
Marian Malloy: Absolutely, yes.
Julie Chen: Dr. Bernstein, Marian Malloy, thank you both for coming on the show talking about this.


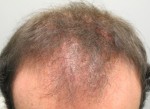 LPP in Male Pattern Alopecia
LPP in Male Pattern Alopecia
 Dr. Eric S. Schweiger, board-certified dermatologist, is quoted in a few recent articles on the effects of chemotherapy on hair, genetic testing for hair loss, and protecting a balding scalp from the sun.
Dr. Eric S. Schweiger, board-certified dermatologist, is quoted in a few recent articles on the effects of chemotherapy on hair, genetic testing for hair loss, and protecting a balding scalp from the sun. O, The Oprah Magazine featured
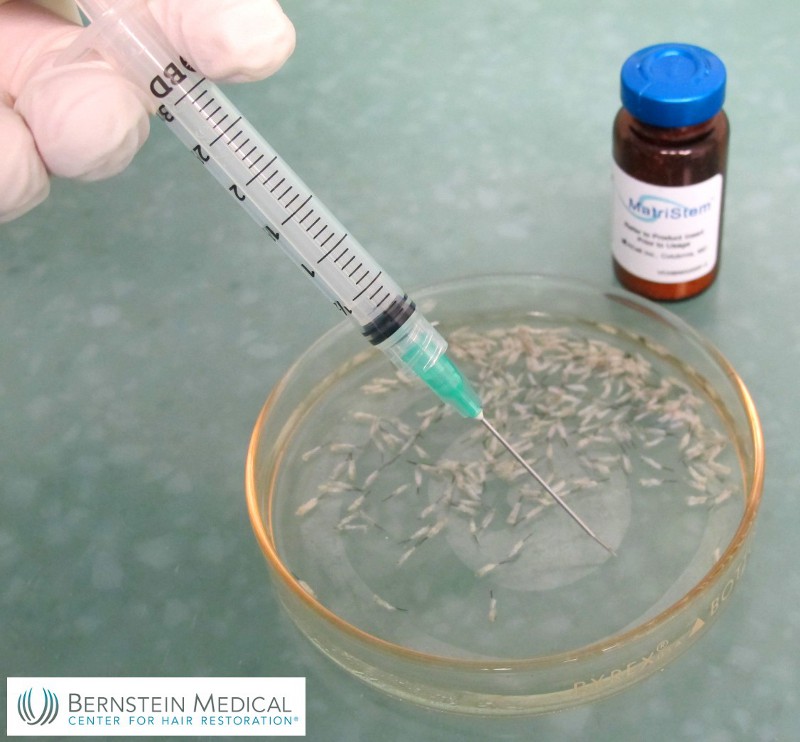
O, The Oprah Magazine featured  The term “follicular unit transplantation” (FUT) has become so firmly embedded in our consciousness that we often consider it synonymous with hair transplantation in general. Surgeons new to the field may be unaware of its origin and how the concept evolved. In the 1980s, many separate clinics were developing total micrografting techniques to improve the naturalness of hair transplantation. In 1988, Dr. Bobby Limmer began developing a technique consisting of single strip harvesting with stereomicroscopic dissection of the hair follicles within the strip, which he published in 1994.
The term “follicular unit transplantation” (FUT) has become so firmly embedded in our consciousness that we often consider it synonymous with hair transplantation in general. Surgeons new to the field may be unaware of its origin and how the concept evolved. In the 1980s, many separate clinics were developing total micrografting techniques to improve the naturalness of hair transplantation. In 1988, Dr. Bobby Limmer began developing a technique consisting of single strip harvesting with stereomicroscopic dissection of the hair follicles within the strip, which he published in 1994. In a new article appearing on the cover of Hair Transplant Forum International, the official publication of The International Society of Hair Transplant Surgeons (ISHRS), pioneering hair transplant surgeon Robert M. Bernstein MD, along with his colleague Dr. William R. Rassman, recently revealed details about a “New Instrumentation for Three-Step Follicular Unit Extraction.”
In a new article appearing on the cover of Hair Transplant Forum International, the official publication of The International Society of Hair Transplant Surgeons (ISHRS), pioneering hair transplant surgeon Robert M. Bernstein MD, along with his colleague Dr. William R. Rassman, recently revealed details about a “New Instrumentation for Three-Step Follicular Unit Extraction.”
 Some of the world’s most renown hair transplant surgeons gathered this month to hear about the latest cutting edge methods in surgical hair restoration. Speakers included Robert M. Bernstein. M.D. founder of Bernstein Medical – Center for Hair Restoration, New York, NY
Some of the world’s most renown hair transplant surgeons gathered this month to hear about the latest cutting edge methods in surgical hair restoration. Speakers included Robert M. Bernstein. M.D. founder of Bernstein Medical – Center for Hair Restoration, New York, NY

 “Hair doesn’t grow singly it grows in naturally occurring groups of from one to four hairs. In follicular transplantation, we use these naturally occurring groups as the unit of the transplant,” he told CST.
“Hair doesn’t grow singly it grows in naturally occurring groups of from one to four hairs. In follicular transplantation, we use these naturally occurring groups as the unit of the transplant,” he told CST.