The principle behind hair transplantation is quite simple. The hair that grows on the back and sides the scalp tends to be permanent in most individuals. It persists even in advanced degrees of androgenetic hair loss because follicles in these locations are not subject to the affects of the hormone dihydrotestosterone (DHT).
The resistance or susceptibility of individual hair follicles to DHT is a genetic characteristic of that follicle and remains with the follicle even if transplanted from one part of the scalp (or body) to another. Therefore, permanent hair transplanted to a bald area will continue to grow at its new location. This phenomenon is termed “donor dominance” because the hair maintains the DHT resistant characteristics of the area where it came from (also called the donor area).
Interestingly, not all of the characteristics of hair are controlled by the genetics of the hair follicle. Wave, for example, is determined by the surrounding scalp, rather than by the follicle per se, so that straight hair transplanted from back of the scalp to the front will become wavy after a hair transplant, if the original hair in the front of the scalp was wavy.
The rate of hair growth and the ultimate length of the hair are affected by both the hair follicle and the skin that surrounds the transplanted hair. Therefore, slowly growing leg hair transplanted to the scalp will grow faster and longer on the scalp, but will not reach the length or thickness of the original scalp hair. The length of scalp hair transplanted to the eyebrow will decrease over time, but will most likely always need to be trimmed.
It is important to understand that in a hair transplant, permanent hair is redistributed to cover the areas of the head where the hair has thinned or has been lost. In hair transplantation surgery, no new hair is actually created – existing hair is just moved around, so there is no net increase in hair. In spite of this, a skillfully performed hair restoration procedure can make a person “look” as though he or she has more hair – often considerably more. In addition, a hair transplant by an experienced hair restoration surgeon will look totally natural with the transplanted hair continuing to grow for one’s lifetime.
The amount of permanent donor hair a person has is a major factor in determining which people are good candidates for a hair transplant. It affects every aspect of the surgical planning and determines how full the results can potentially be. Therefore, a careful assessment of a person’s available donor supply is extremely important in the hair transplant evaluation. The most accurate way for the donor area to be evaluated is through a densitometer or video-microscope – instruments that allow the hair transplant surgeon the ability to examine hair follicles under high power magnification.
In theory, when it is possible to clone hair, the limitations of the donor supply will disappear. In this case, persons with common baldness will not only be candidates for hair transplantation, but will be able to achieve almost any degree of fullness desired. Until this time, however, the finite nature of a person’s donor supply must always be kept in mind.
The process of hair restoration is both an artistic endeavor and a technical feat. The physician must create a natural looking result that is consistent with the available hair supply, the person’s specific hair characteristics, and the patient’s goals. One must design a hair transplant that will not only look good today, but be appropriate as the person ages. But art alone will not ensure a successful hair transplant. The movement of thousands of tiny grafts requires tremendous technical skill; therefore, a highly trained, experienced, clinical support staff is crucial when performing these long, organizationally complex procedures.
The physician must have an in-depth knowledge of the anatomy and physiology of human hair and scalp and have a complete understanding of the medical conditions that affect the scalp. The hair transplant surgeon must also know facial anatomy, possess excellent surgical skills and have a thorough knowledge of the different hair restoration procedures and reparative techniques. The best physicians must be committed to keeping abreast of the new developments in the field – or be directly involved in developing them. Preferably, the physician should devote the majority of his or her clinical practice to this highly demanding sub-specialty. It is literally impossible for the casual practitioner to perform state-of-the-art hair transplant surgery.
History
Reports of successful hair transplants appeared in the early 1930s in Japanese medical literature for the treatment of various types of hair loss of the scalp, eyebrows and moustache, as well as increasing hair in the female pubic area. In the course of developing their procedures, the Japanese physicians made a number of important observations. These included; noting that smaller grafts produced better cosmetic results than larger grafts, that the donor hair was best removed with a single, long incision that could be sutured closed, that the recipients sites (holes in which the grafts are placed) should be made with a needle, and that grafts would survive best if stored in normal saline (similar to the salt concentration of human serum). They even observed phenomenon called telogen effluvium – the annoying shedding of hair that may accompany hair transplant procedures even today. Most importantly, they demonstrated that single-hair grafting resulted in growth that was almost indistinguishable from naturally grown hair.
Unfortunately, because of the poor communication of scientific knowledge between the East and West, further exacerbated by WW II, it would be many decades before Western surgeons would apply these important insights to their own hair restoration procedures.
The first hair transplant in the United States was performed by Dr. Norman Orentreich in 1952. At first, the results of his research were rejected by the editors of several prestigious medical journals, due to their disbelief that such a procedure was possible. Ultimately, his work was published in the Annals of the New York Academy of Science in 1959. In his paper, he explained the concept of “donor dominance” – the idea that grafts continue to show the characteristics of the donor site after they have been transplanted to a new site. This remains the basic concept that underlies all hair transplant procedures.
Yet while donor dominance insured that transplanted hair could grow, it did not guarantee that the results would look natural. In Dr. Orentreich’s original procedures, he used grafts measuring 6- to 8-mm in diameter. He picked grafts this size thinking that those larger than 6-8 mm would not allow sufficient oxygen to reach the center of the grafts (causing the hair at the center not to grow) and he felt that smaller grafts would not contain enough hairs to make the procedure worthwhile. (He later settled on 4-mm as the ideal graft size.)
In Dr. Orentreich’s original work, and for most of the hair transplant procedures performed until the early 1980s, grafts were obtained using an instrument called a trephine or punch. This small, round, cookie-cutter like instrument, removed a cylinder of hair-bearing tissue from the back of the scalp. The same instrument was then used to make a hole in the bald scalp where the graft was to be inserted. The punch made a circular incision in the bald scalp, and then the core of hairless tissue was removed and replaced with the hair-bearing tissue obtained from the permanent zone in the back of the scalp.
 The “punch instrument” used in early hair transplant procedures.
The “punch instrument” used in early hair transplant procedures.By the 1980s, the standard graft size was reduced to 3- to 3.5-mm, significantly smaller than the original sizes described in the 1959 paper, but still large enough to produce a poor cosmetic outcome for the majority of patients. The infamous “pluggy, baby-doll look, so characteristic of the older procedures was the consequence of using these large grafts.
 A large graft from the early days of hair transplantation was almost the size of a pencil eraser.
A large graft from the early days of hair transplantation was almost the size of a pencil eraser.The older procedures would generally involve the transplantation of perhaps 25 to 50 grafts in a one to two hour procedure. A series of these procedures was often planned, with each hair transplant session spaced several months apart to allow for healing. The healing from these large plugs, meanwhile, was slow. The patient left the office in a large turban-like bandage that was kept on for several days. Once removed, the patient had thick adherent scabs that persisted for weeks. The patient also frequently experienced significant amounts of post-operative bleeding.
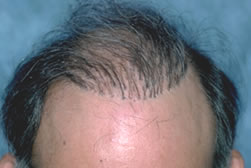 The pluggy look typical of the older hair transplant procedures that resulted from using grafts that were too large.
The pluggy look typical of the older hair transplant procedures that resulted from using grafts that were too large.In an effort to make these large graft hair transplants less pluggy and more cosmetically acceptable, doctors started to use smaller punches. The problem was that the smaller punches caused more damage to the grafts. The reason was that it was hard to line-up the smaller punches with the angle of the hair. With the smaller punches, even a small deviation from parallel resulted in a significant amount of damage to the hair.
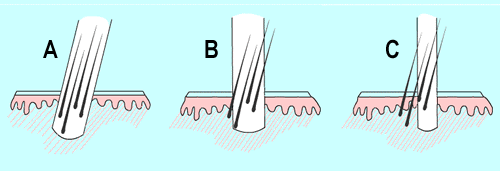 The poor alignment of the punch in (B) causes the lower part of the follicles to be cut off. With a smaller punch (C), the effect is even more dramatic with significantly more damage to the grafts.
The poor alignment of the punch in (B) causes the lower part of the follicles to be cut off. With a smaller punch (C), the effect is even more dramatic with significantly more damage to the grafts.Eventually realizing that the punch-type harvesting technique of any size produced a lot of damage to hair follicles (and also left open wounds in the back of the scalp that bled after the procedure and took weeks to heal) doctors began to remove donor tissue from the back of the scalp in thin, long strip. The open area was then sutured closed, resulting in one, long fine incision. The new procedure was called strip-harvesting in contrast to the older, open-donor technique.
Because it was difficult and time consuming to obtain grafts from a single strip of donor tissue, doctors developed an instrument called a multi-bladed knife that enabled them to harvest (remove) the donor tissue in multiple, thin, long strips. The multi-bladed instrument contained up to 8 blades and could harvest as many as 7 strips at one time each several millimeters in width. The strips could measure as long as 30 or more cm in length.

Multi-bladed knife
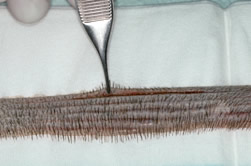
Long, thin strips produced by multi-bladed knife
The thin strips were then cut into smaller pieces containing up to approximately 6 to 8 hairs (called mini-grafts or slit-grafts) and were placed into pre-made sites in the bald area. These recipient sites were made either with the old punches that removed a cylinder of tissue to make room for the new grafts or with a scalpel that produced a small slit that the graft was inserted into. The hair transplants performed in this manner were called “mini-grafting” or “slit-grafting.”
It was soon realized that even these smaller grafts looked quite unnatural, particularly at the frontal hairline. For this part of the restoration, it was necessary to use only 1- and 2-hair grafts. These grafts were obtained by cutting up the mini-grafts into smaller parts. The 1- and 2-hair grafts were called “micro-grafts” and the procedure where 1- and 2-hair grafts were used at the hairline and 3- to 8-hair grafts were used in other parts of the scalp became known a mini-micrografting.
Despite the fact that mini-micrografting techniques were a significant improvement over the older punch-graft techniques, there were many problems with the procedure. The main one was that the procedure still did not look completely natural. In patients with very light hair, or if the patient combed his hair to the side, the results might be acceptable; however, if the patient had dark or coarse hair, or he wanted to comb his hair back exposing his hair line, the hair transplant was obvious.
The second major problem was that the use of a multi-bladed knife actually destroyed hair. The multiple blades cut though hair follicles causing damage to the tissue and poor growth. The result was a decreased supply of viable hair and an unnecessarily thin look to the hair restoration.
It was a slow evolution, but the large grafts used throughout the sixties and seventies eventually gave way to mini-grafts in the eighties and mini-micrografting in the early nineties. The stage was then set for Follicular Unit Transplantation. First described by Bernstein and Rassman in 1995, it quickly emerged as the state-of-the-art in hair restoration, supplanting mini-micrografting in the treatment of androgenetic hair loss and rendering other well-established procedures such as scalp reductions, scalp lifts and flaps virtually obsolete. The next chapter will be devoted to describing this revolutionary hair transplantation technique.
What is a Hair Graft?
During a hair transplant, small grafts of skin containing hair follicles are removed from the areas of permanent hair in the back and on the sides of the scalp, and moved to the areas of thinning or complete baldness. The grafts are placed into small openings created in the bald areas using a fine needle, scalpel or other fine instrument. The openings can be created using various instruments and may consist of needle holes, small slits (incisions where tissue is not removed), punch holes, or laser made holes (where recipient tissue is actually removed or destroyed to provide room for the graft).
As discussed above, both the size of the grafts and the size of the recipient sites have become smaller over the past 40 years. This decrease in size has made the transplants dramatically more natural in appearance.
Grafts can survive for a variable time outside the body depending upon how they are handled and stored. From the time the hair bearing tissue is removed from the back of the scalp, until the time it is placed back in the balding areas it must be kept in a cool, damp environment to insure maximum survival. With large hair transplant procedures of long-duration, proper graft handling and storage is particularly important.
Because grafts are transplanted from one part of the body to another (an “autograft”) rather than from one person to another (an “allograft”), the grafts are not rejected by the body. This had two important implications; first, the doctor does not generally need to test a person to see if a hair transplant will work and second, no medications are needed to insure the growth of the transplanted hair. This is in stark contrast to allografts (such as kidney or liver transplants) where the person receiving the transplant must remain on powerful immune suppressing drugs to prevent its rejection by the body.
Graft Sizes
Grafts are usually divided into five general categories: standard punch grafts, minigrafts, slit grafts, micrografts, and follicular unit grafts. Standard punch grafts are 3-4 mm in diameter and each may contain up to 30 hairs (and 10 or more intact or partial follicular units). Minigrafts are smaller, 1.2-2.5 mm in diameter, and have 4-12 hairs per graft. Slit grafts are similar in hair content to mini-grafts but are rectangular in shape, rather than round, due to the fact that they are cut from long, thin strips (rather than being removed from the scalp with a punch). Micrografts are even smaller, measuring 1.5-1.0 mm or less in diameter, with 1-2 (or 3) hairs per graft. Follicular unit grafts are composed of single follicular units. These naturally occurring groupings may contain from 1 to 4 hairs each.
Small Grafts vs. Large Grafts
Large grafts placed in a frontal hairline look pluggy and unnatural when the hair was combed back or to the side. With the older procedures, the hair transplant patient was forced to comb his hair forward to hide his hairline. To create more natural looking hairlines, physicians began decreasing the size of grafts and began placing these smaller grafts in front of the larger ones. The problem was that the larger grafts were visible if the hair was not perfectly groomed and other areas of the scalp would not look natural, particularly if the patient continued to lose hair.
The use of larger grafts also obligated the patient to have multiple hair transplant sessions in order to have even modestly decent results, with the patient’s appearance often being strikingly unnatural before the restoration was completed. Even with additional work, the large graft transplants often fail to appear natural because they are intrinsically clumpy. On close inspection, it is literally impossible for large graft transplants to look and feel natural, even after the best work.
It became apparent that using all smaller grafts would be preferable, but the amount of time and work needed to transplant large number of very small grafts was much greater than the effort needed to transplant a smaller number of larger grafts. Also, smaller grafts were more easily damaged during the dissection and placing process and special skills were needed to handle them effectively. Although small mini-grafts and micrografts looked more natural, they resulted in significant damage to the follicles. It wasn’t until the introduction of stereo-microscopic dissection and special placing techniques used in the follicular unit hair transplant procedure that these problems would be solved.
As a cautionary note, some hair transplant surgeons invent unusual terms for grafts in an attempt to make it appear that they have some special, unique knowledge or technique. Do not be confused by fancy terminology. The potential patient should be wary when a doctor claims to have a unique technology or technique that no other doctor knows about or uses. Worthwhile procedures will be documented and published in peer-reviewed medical journals.
Methods of Harvesting Grafts
There are a number of methods commonly used to harvest grafts. The original one, devised by Dr. Orentreich, uses a hand operated punch to cut single grafts that were 4-mm in size and contained up to 30 or more hairs. Besides producing very large grafts, there was significant hair wastage due to the destruction of hair follicles around the perimeter of the punch. As described in the history section, this problem was exacerbated if the punch was not perfectly aligned with the hair follicles and made even worse when the punches were reduced in size. A variation of this method utilizes a motorized punch that rotates at high speeds with the same, poor result.
The large grafts obtained by punch methods can be made into minigrafts by cutting them into halves or quarters. The donor area can be closed by suturing or can be left open – the more common technique since the former was very tedious. If the donor sites are not closed, they develop significant round white scars that can become visible later in life. Most doctors have abandoned using these techniques.
Another method uses a series of scalpel blades attached in parallel on a handle, called a multi-bladed knife. This instrument generates multiple thin strips of hair-bearing donor tissue which are subsequently cut into smaller pieces. This method is fast and still quite popular. Unfortunately, this method can cause extensive damage to the donor tissue, as it is impossible to line up the multiple blades parallel to the hair follicles. In a fourth method, called single strip harvesting, the donor tissue is removed as a single, long, thin strip. The great advantage of this method is that the tissue is removed from the scalp with the minimal amount of damage. Further dissection is then performed using a dissecting stereo-microscope. This technique keeps potential injury to follicles to an absolute minimum and allows preservation of intact naturally occurring follicular units – it is the technique used in Follicular Unit Transplantation procedures.
All donor “harvests” result in a scar but, if done properly, the scar from the hair restoration procedure should be undetectable. Not only is it important for the scar to be closed meticulously – so that it will be as fine as possible – but the incision must be placed in the proper location, so that it will remain covered with hair even with further balding. Scars that are placed very high on the back or sides of the scalp, run the risk of being visible if there is extensive balding. In addition, the hair that is obtained from high positioned incisions may not be permanent. Scars that are place too low have an increased risk of stretching from the movement of the neck muscles transmitted to the scalp.
Removing the old scar in subsequent hair transplant procedures is important for two reasons. First it keeps the second incision will positioned within the permanent zone of hair and second, it leaves the patient with just one scar in the donor area. Some doctors harvest a new area for each surgery. When many surgeries are done, these patients have a stepladder appearance of the back of the scalp from the multiple procedures – a situation that can easily be avoided.
Appearance of Hair Transplants
A hair restoration procedure is particularly bad when everyone can tell it is a hair transplant. The uneven, patchy effect of the large pluggy grafts occurs when large grafts are used and the spaces between the grafts are wide. This causes a contrast between the bald skin and the islands hair scattered over it creating the infamous “dolls-head” appearance.
Traditional hair transplants also produce small subtle changes in the skin. With larger grafts, the surface of the transplanted skin may not be aligned with the surface of the surrounding scalp leaving slight irregularities when they heal. The base of larger grafts may also take on a white scarred appearance that can be permanent. As the graft size decreases, these changes become less obvious. With follicular units these surface change can be completely avoided.
However, even with the use of very small grafts, hair transplants can still look unnatural. Hairline placement and proper hair direction are critically important to the natural outcome of the procedure and the skill to perform this with absolute perfection is possessed by only a few of the most talented hair restoration surgeons.
Hairlines
The design and position of the hairline are perhaps the most critical aesthetic aspect of the hair restoration. Some physicians create the same standard hairline on every patient; however, natural hairlines vary greatly from one individual to another. The hair transplant surgeon must be acutely aware of the spectrum of variations that normally occur and tailor each hairline to the patient’s specific facial features. He must also take into account that, as the patient matures his facial features will change and he will continue to bald, but the position of the transplanted hairline will be permanent.
Few natural hairlines are symmetrical; therefore, one should not attempt to create a perfectly balanced hairline, as it is distinctly unnatural looking. Errors can occur when over-demanding patients or over-aggressive doctors place the hairline too low on the forehead, or restore the juvenile (adolescent) hairline. Although it is important that the patient play and active role in decisions regarding the placement and design of the hairline, it is up to the physician to educate the patient and set the parameters to insure that the procedure will look natural, now and in the future.
Hair and Its Variations
Certain hair types may be more common in certain human groups. Understanding these characteristics may be critical in anticipating the results one can expect. African hair is very curly. This single characteristic makes African hair produce some of the best results in hair transplantation, but the dissection must be performed with extreme care to avoid damage to the curved follicles.
Most Asian hair is black, coarse and straight, making it critical that a deep zone of one-hair grafts are used at the hairline to insure a natural look. The use of the stereo-microscope can insure that only single units are placed in this area. Using only naturally occurring individual follicular units will produce natural results with all hair and skin types.
Hair grows in different directions in different parts of the scalp. Hair in the front and top of the scalp grows predominantly forward; hair in back of the scalp grows downward; hair on the sides of the head grows away from the middle. The place where the hair changes from the forward direction to the back is called the vertex transition point and is more commonly know as the crown. In designing the hair transplant, your surgeon should have a knowledge of these natural growth patterns, your hairstyle preferences, and how you want your hair to look when you hair is both groomed and un-groomed. A thorough understanding of all the nuances of the different hair characteristics and patterns that individuals may possess is essential in producing consistently superior results.
Continue reading: Chapter 8 – Follicular Unit Transplantation »»
Table of Contents
| Introduction | |
| Chapter 1 | Brief History of Hair |
| Chapter 2 | Hair and Its Functions |
| Chapter 3 | Causes of Hair Loss |
| Chapter 4 | Hereditary Baldness |
| Chapter 5 | Psychology of Hair Loss |
| Chapter 6 | Hair Loss Medications |
| Chapter 7 | Hair Transplant Basics |
| Chapter 8 | Follicular Unit Transplantation |
| Chapter 9 | Follicular Unit Extraction |
| Chapter 10 | Master Plan for Restoring Hair |
| Chapter 11 | Goals and Expectations |
| Chapter 12 | Numbers of Grafts Needed |
| Chapter 13 | Hair Transplant Repair |
| Chapter 14 | Hair Loss in Women |
| Chapter 15 | Hair Systems and Camouflage |
| Chapter 16 | Preparing for a Hair Transplant |
| Chapter 17 | The Hair Restoration Procedure |
| Chapter 18 | What to Expect Following Surgery |
| Chapter 19 | Hair Transplant Fallacies |
| Chapter 20 | Choosing Your Doctor |
| A Final Note | |
| References | |
| About the Author |





