Robert M. Bernstein, M.D.
Hair Transplant Forum Intl. 2012; 22(6): 228-229.
I began performing FUE in the late 1990’s although, at the time, it was a very small part of our practice. When Dr. Rassman and I wrote the first paper on Follicular Unit Extraction in 2002 (the paper which gave FUE its name), we stressed the difficulty of harvesting intact follicular units using a hand-held punch. ((Rassman WR, Bernstein RM, McClellan R, Jones R, et al. Follicular Unit Extraction: Minimally invasive surgery for hair transplantation. Dermatol Surg 2002; 28(8): 720-7.)) We found such great variability in the transection rate between patients that we recommended performing a test (the Fox Test) prior to scheduling the actual procedure. This was done in order to distinguish between good surgical candidates and those patients where the risk of follicular damage would be too great to make the surgery practical.
After trying a variety of different instruments and techniques, a major breakthrough came with Dr. Harris’ idea to use a three-step technique. With this method, a sharp-punch was used to score the skin and then a dull punch was used to go deeper and separate the follicular units from the surrounding tissue. The third step was the actual extraction using forceps, so we now simply refer to it as the 2-step technique. Using a dull punch for the dissection in step two allowed us to minimize injury to the follicles. However, there was still a relatively high incidence of buried grafts when the sharp instrument was removed and the dull instrument inserted, pushing the grafts into the subcutaneous space. ((Harris JA. The SAFE System: New Instrumentation and Methodology to Improve Follicular Unit Extraction (FUE). Hair Transplant Forum Intl. 2004; 14(5): 157, 163-4.)), ((Bernstein RM, Rassman WR. New Instrumentation for Three-Step Follicular Unit Extraction. Hair Transplant Forum International 2006; 16(1): 229, 237-9.)), ((Rassman WR, Harris J, Bernstein RM. Follicular Unit Extraction. In: Haber RS, Stough DB, editors: Hair Transplantation, Chapter 17. Elsevier Saunders, 2006: 133-137.))
The logistical problem of using two distinct steps was cleverly addressed by Jim Harris with his powered, hand-held device. A single, rotating punch acted as a sharp instrument (when rotating quickly) and then as a blunt instrument (as it rotated more slowly). ((Harris JA. Powered blunt dissection with the SAFE System for FUE Part I. Hair Transplant Forum Intl. 2010; 20(6): 188-189.)) The elegance of the instrument was that, as the punch advanced deeper into the skin, the friction on the punch from the surrounding skin would automatically slow the rotation so that only the initial, entry-speed adjustment had to be made.
In our experience, this instrument decreased the incidence of both transection and buried grafts. Problems remained, however, as a number of patients still had unacceptable rates of transection, particularly those with finer hair and very loose scalps. Another issue was that as FUE sessions grew larger (and longer); it became increasingly difficult to achieve consistent results due to human error and fatigue.
Benefits of Robotic FUE
The first step in FUE, namely, the separation of the follicular units from the surrounding donor tissue, is a highly repetitive and labor intensive process that requires great precision. This step requires centering the punch over the follicular unit and aligning the dissecting instrument with the follicles/follicular units, in order to prevent damage. This step, which must be repeated hundreds to thousands of times in a typical FUE hair restoration procedure, is the step that is most subject to human variability and error. In my opinion, it is the step that most readily lends itself to automation.
The first robotic system for FUE became commercially available in late 2011. ((ARTAS™ System manufactured by Restoration Robotics, Inc. (Mountain View, CA).)) It uses an image-guided robotic device to separate follicular units from the surrounding tissue for subsequent extraction. The advantage of using a robot to minimize human error is obvious, but the new system also uses a combination of sharp punch and blunt dissection – the technique that we found worked best with the hand-held devices. Additionally, it allows us to remove grafts with forceps, rather than by suction. This feature is important since strong suction, in my opinion, can be damaging to grafts. It was these two reasons that prompted us to introduce the technology into our practice in November 2011. We now perform the majority of our FUE cases using this robotic system (see Figure 1.).
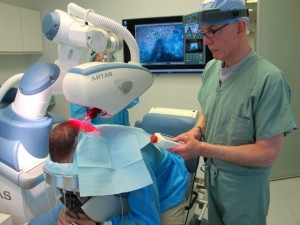
Figure 1. Robotic device used at Bernstein Medical – Center for Hair Restoration.
The robotic system is composed of a computer, a mechanical arm, a punch mechanism, a video-imaging system and a user interface. Its dissection technique is enabled by two punches which are concentrically arranged – a small diameter, sharp bi-beveled punch is nested within an outer, dull punch. The inner punch has cutting capabilities to score the upper most part of the skin and the outer punch has a blunt edge that dissects the follicular units from the surrounding tissue, minimizing injury to the grafts.
We find that the consistency in performing this task thousands of times without its accuracy waning from fatigue is a main benefit of using a robot for follicular unit extraction. We have also found that grafts harvested with robotic FUE showed less transection (compared to a hand-held device) and contained more of the surrounding protective tissue, particularly around the lower portion of the follicular unit. One would assume that the better quality grafts will lead to increased graft survival; however, this has not yet been tested in controlled studies.
We find that the robot is more versatile in its ability to harvest grafts from patients with different hair characteristics and from different parts of the scalp. Although there is still variability in the ease of extraction among patients of different racial backgrounds, in our experience, the differences are less when compared to a hand-held system. Also, with the robotic system it seems easier to extract grafts from the sides of the scalp where the hair angle is more acute.
The robotic system reduces harvesting time, particularly in larger sessions where doctor and staff fatigue tends to set in. While a hand-held device requires great effort to perform sessions greater than 1,500 grafts, we are now able to comfortably extract 2,000 grafts in one day and over 2,500 grafts in two consecutive days. ((Bernstein RM, Rassman WR. Anderson KW. Follicular Unit Extraction Megasessions: Evolution of a technique. Hair Transplant Forum International 2004; 14(3): 97-99.))
Modifications to the Robotic System
The initial version of the robot required real-time adjustments in parameters such as the depth and angle of the punch and the speed of rotation. Although the imaging system of the robot allowed these changes to be made quite easily, there were a fair number of adjustments to monitor. It is a bit too technical to detail all the modifications in this brief discussion, but the result is a system that requires far less human intervention than with earlier iterations. The user interface has also been improved and automatic features added, so that the new version makes the robot much easier to operate compared to the older ones.
One of the main modifications I made to the system was to decrease the diameter of the sharp punch from 1.0mm to 0.9mm (with a concomitant decrease in the size of the blunt punch). This decreases the wounding to the donor area, facilitates healing and increases the number of grafts that can be obtained per unit area by approximately 30%. In our experience, it also produces grafts that are “ready-made” for implantation, as grafts from the updated system require little or no trimming under the stereo-microscope prior to insertion.
There are several additional changes being made to the robot system to make it more practical. Currently, the patient can only lie on the robotic device face-down. While this position is necessary for the robotic arm to have full access to the donor area, it does not allow easy access to the front or top of the scalp. As a result, graft placement must be performed using a separate operating chair, necessitating the use of two operating rooms for one patient. Fortunately, we have the space at our center, but many offices, particularly those in large cities, do not have this much room available. Within a year, the robotic operating table will be re-designed so that harvesting and placing can be performed in the same room, eliminating this constraint.
One of the things that slow down the robotic process is the tensioner mechanism used to stretch the scalp. Although this feature has the advantage of decreasing follicular transection, it must be removed and applied to a new area every 100 to 150 grafts. With a larger and easier to use tensioner (which has already been designed), the delay from its re-positioning should be significantly decreased.
The robot harvests grafts in a square field. When one field is finished, the tensioner is manually advanced to the next area. With slight overlapping, one field can be made to imperceptibly blend into the next. However, the two ends of the harvested donor area have a squared-off look that persists until the donor area completely heals. The outside edges can be gently feathered to produce a softer look, but this takes a little time for the surgeon using the current available tools in the software. A more automated algorithm is being developed and will be deployed in future versions of the software.
Integrating Robotic FUE into the Practice
Soon after we began using the robotic device, and were able to appreciate its benefits, I stopped using the hand-held system for all but the smallest FUE cases. The major changes that we made after integrating robotic FUE into our practice were related to performing the larger sessions of FUE permitted by the new technology. Although the ability to harvest a greater number of grafts in one sitting is clearly an advantage, having grafts outside the body for an extended period of time can be detrimental to their growth. It is also physically difficult for both the patient and staff when procedures last significantly longer than eight hours.
In Follicular Unit Transplantation (FUT), follicular units are obtained through the stereo-microscopic dissection of a harvested donor strip. Since this process takes place on a dissecting table, graft dissection can proceed simultaneously with site creation and graft placement. In addition, the dissection can be done by multiple dissectors working simultaneously to complete the process quickly. In FUE, however, individual follicular units are removed directly from the donor area, making it difficult for site creation and graft placement to be carried out at the same time. This is literally impossible when using a robot for harvesting. In addition, the constraints of the extraction process limit it to being performed one graft at a time, significantly increasing the duration of this step of the procedure. As a result, in FUE procedures, there is a delay from the time grafts are removed from the body until they can be placed into the recipient sites. This delay is, of course, magnified in larger FUE sessions.
To lessen the impact of this interval, we first started using a metabolically optimized holding solution in all of our cases, regardless of their size. This holding solution, which mimics the intra-cellular environment of grafts and soaks up damaging free-radicals, has been shown to increase survival outside the body. It is particularly effective at low temperatures, which we also control for with new digital thermal technology. ((Cooley JE. Ischemia-Reperfusion Injury and Graft Storage Solutions. Hair Transplant Forum Intl. 2004; 14(4): 121, 127, 130.)), ((Cole JP, Reed WM. The optimal holding solution and temperature for hair follicle grafts. Hair Transplant Forum Intl. 2012; 22(1): 17-21. ))
The second change we made to lessen the delay was to simply create all the recipient sites before extracting the grafts. Now, as soon as the grafts are harvested, they can be placed immediately into the recipient scalp. In larger cases, of around 1,800 to 2,000 grafts, we have been pre-making the sites the day before. Not only does this eliminate the delay, but; by allowing the healing process to begin in the recipient area; it minimizes popping, increases visibility due to less bleeding, and possibly creates a more hospitable environment for the newly transplanted grafts. ((Bernstein RM, Rassman WR. Pre-Making Recipient Sites to Increase Graft Survival in Manual and Robotic FUE Procedures. Hair Transplant Forum International 2012; 22(4): 128-130.))
The third change we made was to divide cases over 2,000 grafts into two, consecutive day sessions. This not only takes advantage of pre-making sites (which are all made on day one) in eliminating the site creation delay, but allows large sessions to be performed without placing undue stress on our patients or our staff.
Conclusion
Employing a new device in one’s practice is always a challenging endeavor, particularly when the instrument is as seemingly complicated and bulky as an FUE robot. However, the technical precision and labor intensive processes required for successfully performing large sessions of follicular unit extraction seem to warrant this commitment. Unlike Follicular Unit Transplantation, where the problems of isolating follicular units from a donor strip were solved using stereo-microscopic dissection – even a decade after the widespread adoption of FUE – the challenges of extracting intact follicular units directly from the scalp remain.
We have seen an evolution from sharp punches, to dull punches, to two-step techniques; and from manual punches, to motorized units, to finally an automated device. Whether a robotic system or some other yet-to-be-invented instrument will prove to be the best solution for removing intact follicular units directly from the scalp remains to be determined. However, from this author’s perspective the newly available, image-guided robotic system currently appears to hold the most promise.





